Abstract
Approximately 30% of lymphomas occur outside the lymph nodes, spleen, or bone marrow, and the incidence of extranodal lymphoma has been rising in the past decade. While traditional chemotherapy and radiation therapy can improve survival outcomes for certain patients, the prognosis for extranodal lymphoma patients remains unsatisfactory. Extranodal lymphomas in different anatomical sites often have distinct cellular origins, pathogenic mechanisms, and clinical manifestations, significantly influencing their diagnosis and treatment. Therefore, it is necessary to provide a comprehensive summary of the pathogenesis, diagnosis, and treatment progress of extranodal lymphoma overall and specifically for different anatomical sites. This review summarizes the current progress in the common key signaling pathways in the development of extranodal lymphomas and intervention therapy. Furthermore, it provides insights into the pathogenesis, diagnosis, and treatment strategies of common extranodal lymphomas, including gastric mucosa-associated lymphoid tissue (MALT) lymphoma, mycosis fungoides (MF), natural killer/T-cell lymphoma (nasal type, NKTCL-NT), and primary central nervous system lymphoma (PCNSL). Additionally, as PCNSL is one of the extranodal lymphomas with the worst prognosis, this review specifically summarizes prognostic indicators and discusses the challenges and opportunities related to its clinical applications. The aim of this review is to assist clinical physicians and researchers in understanding the current status of extranodal lymphomas, enabling them to make informed clinical decisions that contribute to improving patient prognosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Approximately 30% of lymphomas arise from sites other than the lymph nodes, spleen or bone marrow [1]. The prevalence of extranodal lymphoma has increased over the past decade [2]. There are two main types of lymphoma exist: B-cell lymphoma and T-cell lymphoma, with B-cell lymphomas being more prevalent than T-cell lymphomas [3]. Common sites of extranodal lymphoma include the gastrointestinal tract, head and neck, skin/soft tissue, central nervous system (CNS) [4, 5]. Different sites of extranodal lymphoma often have unique cellular origins, genetic abnormalities, and clinical behaviour [6].
The diagnosis of extranodal lymphoma necessitates a comprehensive assessment encompassing clinical symptoms, physical examination findings, and laboratory tests. Commonly utilized diagnostic tools comprise imaging studies, such as X-rays, CT scans, MRIs, and PET scans, enabling the identification of the site and extent of lymphoma involvement. Biopsy procedures, including needle biopsies or surgical interventions, are employed to obtain tissue samples, which serve as definitive evidence for lymphoma diagnosis. Immunohistochemistry and genetic tests may be conducted to determine the specific subtype and prognosis of the lymphoma. Furthermore, given the potential involvement of the bone marrow in extranodal lymphoma, a bone marrow biopsy is often performed to evaluate disease spread and facilitate the selection of appropriate treatment strategies. This comprehensive diagnostic approach provides valuable insights into the nature and extent of extranodal lymphoma, aiding in the formulation of effective management plans [7, 8].
The treatment of extranodal lymphoma depends on aspects such as subtype, stage of the disease and the patient's overall health. Conventional treatments include chemotherapy, radiation therapy, targeted therapy, and immunotherapy. Chemotherapy stands as the cornerstone of treatment for the majority of extranodal lymphomas [9] and radiation therapy represents a localized therapeutic modality [10]. In addition, autologous hematopoietic stem cell transplantation (ASCT) may also be an effective salvage measure for extra-nodal lymphoma.
As the diagnosis and treatment of extranodal lymphoma are influenced by its different pathogenesis at different anatomical sites, it is necessary to discuss the pathogenesis of extranodal lymphoma at different sites separately. This review will summarize the common key signaling pathways and intervention treatments in extranodal lymphomas. Furthermore, we thoroughly explore the pathogenesis, diagnosis, and treatment strategies of MALT, NKTCL, mycosis fungoides (MF), and PCNSL, which are the most notable types of extranodal lymphomas occurring in the gastrointestinal tract, head and neck region, skin, and CNS. Besides, considering that PCNSL is one of the lymphomas with the poorest prognosis and there are few articles synthesizing its prognostic indicators, we have comprehensively summarized the prognostic markers of PCNSL and discussed the challenges and opportunities related to clinical applications. This review will contribute to enhancing our understanding of extranodal lymphomas and provide valuable insights for future clinical decision-making.
Signaling pathways and interventional therapy in extranodal lymphoma
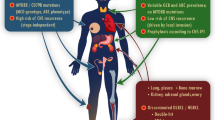
A variety of signaling pathways have been implicated in the pathogenesis of extranodal lymphomas. While different sites of extranodal lymphoma may exhibit distinct signaling pathways, there are still common key signaling pathways shared among them (Fig. 1). These include the NF-κB pathways, Janus-associated kinase/signal transducer and activator of transcription (JAK/STAT) pathways, phosphatidylinositol 3-kinase (PI3K)/ protein kinase B (Akt)/ mammalian target of rapamycin (mTOR) pathway, apoptosis pathway, programmed death-1/programmed death-ligands (PD-1/PD-Ls) pathway, and Cell receptor signaling pathway. Table 1 summarizes the common signal pathway inhibitors currently under clinical investigation for extranodal lymphoma.
NF-κB pathway
The NF-κB pathway is constitutively activated and plays a role in cell survival, proliferation, and immune responses in various types of extranodal lymphoma [11,12,13,14,15]. Both the classical NF-κB pathway, activated by the tumor necrosis factor-α receptor (TNFR) 1, interleukin1 receptor (IL1R), toll-like receptor (TLR), T-cell receptors (TCR), B-cell receptors (BCR), and growth factor receptors (GFR), and the alternative NF-κB pathway, activated by TNFR, CD40 and B-cell activating factor (BAFF), play roles in cell survival, proliferation, inflammation, and immune. In lymphoma, both pathways are constitutively activated and contribute to oncogenic events [16]. Abnormalities in the NF-κB pathway and its upstream or downstream pathways, such as the BCR (B-cell receptor) or TLR pathways, are important mechanisms in the development of lymphomas. Mutations or chromosomal translocations in CARD11, CD79A/B and myeloid differentiation primary response 88 (MYD88) contribute to the activation of the NF-κB pathway [15, 17]. Currently, inhibitors targeting upstream targets of the NF-κB pathway, such as Bruton's Tyrosine Kinase (BTK) inhibitors [18], receptor proximal kinases in NF-κB (like interleukin-1 receptor associated kinase 4 inhibitors) [17] and CD30 inhibitors (typical examples include brentuximab vedotin) [17], have been found to be effective in treating extranodal lymphomas.
JAK/STAT pathway
The JAK/STAT pathway mediates the transmission of signals from cytokines and growth factors. Dysregulation of this pathway has been observed in extranodal lymphomas, including mucosa-associated lymphoid tissue (MALT) lymphomas, natural killer/T-cell lymphoma (nasal type, NKTCL-NT) [13, 19], primary central nervous system lymphoma (PCNSL) [20] and peripheral T cell lymphoma (PTCL) [21, 22]. The JAK/STAT pathway is associated with immune homeostasis, inflammation, cell proliferation, apoptosis and differentiation in extranodal lymphoma [21]. Abnormalities in JAK and STAT have been identified as distinct characteristics of lymphoma. Besides, JAK/STAT pathway may play a role in upregulating PD-L1 and PD-L2 expression in extranodal lymphomas [23]. Inhibitors targeting JAK kinases have shown promising results. The JAK2/FLT3 fusion inhibitor pacritinib has demonstrated preclinical safety and efficacy [22]. The JAK3 inhibitor tofacitinib has shown therapeutic effects in PTCL [24] and NKTCL [19]. A small molecule inhibitor of STAT3 called Stattic can also be effective by inducing apoptosis or inhibiting cell proliferation in NKTCL cells [19]. Targeting the JAK/STAT pathway may provide new treatment options for patients with extranodal lymphomas.
PI3K/AKT/mTOR pathway
The PI3K/AKT/mTOR pathway plays an oncogenic role in extranodal lymphomas. Isoforms p110δ and p110γ belong to the Class I kinase of the PI3K family play a crucial role in the development, proliferation, migration, cytokine secretion, and other cellular functions of B-cells [25, 26], T-cells [26, 27], and NK-cells [28, 29]. Novel PI3K inhibitors (idelalisib, buparlisib, duvelisib and copanlisib) have recently demonstrated promise for the treatment of MALT [30,31,32], PCNSL [33], NKTCL [34] and PTCL [27, 34, 35].
AKT and PTEN are key proteins in the PI3K pathway, acting as positive and negative regulators, respectively. When PTEN is inactivated, it leads to an increase in AKT and mTOR activity, which in turn promotes tumor growth and other pathological changes [17]. Therefore, it is reasonable to target the PI3K/AKT/mTOR pathway for the treatment of PTEN-deficient extranodal lymphomas. Several agents such as AKT inhibitors (MK-2206) [36, 37] and pan-PI3K inhibitor (buparlisib) [38] are under clinical evaluation.
The mTOR is also a key protein kinase in the PI3K/AKT/mTOR pathway, and it serves as a structural unit for mTORC1 and mTORC2 complexes. Upon receiving phosphorylation signals from upstream AKT, activated mTORC1 and mTORC2 carry out their respective functions, positively regulating cell survival, induction of cell cycle arrest, and negatively regulating autophagy [39]. The current focus of research is primarily on first-generation mTOR inhibitors. Among them, temsirolimus and everolimus are typical mTORC1 inhibitors. They can be used alone or in combination with rituximab and have been shown to have favorable efficacy in PCNSL [40, 41], PTCL [42, 43], MZL [40] and NKTCL [44].
Apoptosis pathway
The apoptosis pathway dysregulation in extranodal lymphomas is often due to abnormalities in key regulators like BCL2, p53, and MYC [45,46,47]. For example, upregulation of P53 may inhibit apoptosis in NKTCL [45, 46]. Overexpression of MYC and BCL2 is frequently seen in patients with B-cell extranodal lymphomas [47, 48] and PTCL [49, 50]. BCL2 inhibitors like venetoclax [49] and obatoclax [50] can restore apoptosis. MYC inhibitors and p53 reactivate drugs are being explored. Currently, inhibitors targeting BCL2, p53 and MYC aim to restore apoptosis in lymphoma cells by reactivating programmed cell death mechanisms.
PD-1/PD-Ls pathway
Extranodal lymphoma cells can exploit the PD-1/PD-Ls pathway to avoid immune surveillance by modulating T-lymphocyte activity [51]. PD-1, PD-L1 and PD-L2 were found to be overexpressed in B-cell and T-cell extranodal lymphomas and their tumor microenvironment [52]. The application of immune checkpoint inhibitors in lymphoma is receiving increasing attention. Checkpoint inhibitor antibodies blocking PD-1 (nivolumab, pembrolizumab and Sintilimab) or PD-L1 (atezolizumab, avelumab) have been classified as Level 3 evidence for use in salvage therapy for extranodal lymphoma, including MALT [52], NKTCL [51,52,53,54,55], PCNSL [56], PTCL [52, 54].
Cell receptor pathway
The B-cell receptor (BCR) pathway is a crucial mechanism involved in the immune response. It is characterized by the activation of CD79A/CD79B heterodimers, which transmit antigen-stimulated signals from the cell membrane to the cytoplasm. The persistent activation of BCR pathway relies on the phosphorylation of immunoreceptor tyrosine-based activation motifs by Src family kinases, leading to the recruitment and activation of spleen tyrosine kinase. This activation triggers downstream signaling pathways, including PI3K/AKT/mTOR, NF-κB, and MAPK. CD79A/B and BTK play critical roles in this process, and their dysregulation has been implicated in B-cell extranodal lymphoma such as PCNSL [57, 58], MALT [59, 60]. Inhibition of BTK, with drugs like ibrutinib, has shown promising efficacy against these malignancies by disrupting BCR pathways and downstream NF-κB pathways.
The T-cell receptor (TCR) plays a key role in the pathogenesis of PTCL by providing "signal 1" through engagement with antigen peptides presented on major histocompatibility complex (MHC) molecules for lymphoma cell growth and survival [61]. Targeting TCR signaling, like Src family kinase inhibitors dasatinib is effective in treating PTCL. Dasatinib demonstrated an overall response rate of 29% in relapsed/refractory PTCL [62]. However, no TCR pathway inhibitor drug has been approved by the FDA. This may be due to the fact that the efficacy and safety of TCR pathway inhibitors require further study [63].
Gastric mucosa-associated lymphoid tissue Lymphoma
Pathogenesis
Gastric lymphoma is the most common form of extranodal lymphoma, accounting for 30–40% of all extra-nodal lymphomas. Histopathologically, MALT lymphoma is the most common primary gastric lymphoma subtype [64].
The majority of patients (80–90%) with gastric MALT lymphoma are infected with H. pylori (HP) [65]. The development of gastric MALT lymphoma is closely associated with HP-mediated regulation of T cells, HP-induced cytokines and chemokines, HP antigen stimulation, and s mediation of signaling molecules. T-cell responses induced by HP infection play a critical role in tumor growth and progression. In the early stages of gastric MALT lymphoma development, HP-stimulated infiltrating T cells promote the proliferation and differentiation of B lymphoma cells. This process involves CD40 signaling, secretion of Th2-type cytokines (such as interleukin-4, interleukin-5 and interleukin-10) upon exposure to HP antigens [66]. Moreover, alterations such as the loss of CXCR4 [67] and upregulation of CXCR7, BCA-1 and its receptor CXCR5 [68] are also involved in the development of gastric MALT lymphoma. Activation of phospho-Src homology-2 domain-containing phosphatase and HP CagA-mediated signaling molecules further promote B-cell proliferation [69]. Chronic infection often contributes to gastric MALT lymphoma by inducing aberrant B cell survival and proliferation through BCR pathway [70]. PI3K pathway is critical for the proliferation and survival of malignant B cells [71]. Interestingly, HP-negative MALT lymphomas have shown a high frequency of positive t(11;18) (q21;q21) [72]. This translocation event leads to the formation of a fusion protein called API2-MALT1, which in turn activates the transcription factor NF-kappa through enhanced IKK gamma polyubiquitination [73]. The above findings suggest that t(11;18)(q21;q21) may be a major contributor to the development of gastric MALT lymphoma and is associated with a poor prognosis [73].
Diagnosis
In addition to routine physical examinations, blood tests, biochemistry, enhanced whole-body CT scans, and endoscopy can also be used as part of the pre-treatment evaluation of gastric MALT lymphoma. Endoscopy is an indispensable tool for the initial diagnosis and follow-up of gastric MALT lymphoma cases and for obtaining biopsy specimens [74]. The urea breath test can rapidly detect the presence of HP infection and can also assist in the repeated evaluation of the effectiveness of anti-HP treatment [75]. HBV [76] and HCV [77] testing not only aids in the diagnosis of certain types of gastric MALT lymphoma but may also serve as a therapeutic target. Gastric MALT lymphoma diagnosis depends on pathological diagnosis and all pathological specimens should be routinely tested by immunohistochemistry (IHC). The typical immunophenotypes of gastric MALT lymphoma are CD5-, CD10-, CD20 + , CD21-/ + , CD23-/ + , CD43-/ + , cyclin D1- and MNDA ± [8]. Detection of the translocation should also aid in the clinical management of patients with gastric MALT lymphoma. HP-negative gastric MALT lymphoma can be detected by reverse transcription-PCR or FISH and (t 11;18) is often indicative of advanced disease and poor anti-HP efficacy [78].
Treatments
Anti-HP therapy is highly recommended for patients diagnosed with limited gastric MALT lymphoma and confirmed positive for HP infection [79]. Anti-HP therapy results in remission in 60–80% of patients, even in HP-negative patients [65]. For patients who are t(11;18)(q21;q21) positive, have residual tumors after anti-Hp therapy, experience symptoms such as concurrent bleeding, or are not suitable candidates for HP treatment, radiotherapy is frequently employed as a salvage treatment [78, 80]. Rituximab in combination with chemotherapy is the usual treatment modality for stage III/IV gastric MALT lymphoma that has failed local radiotherapy without B symptoms, bleeding, blood cell depletion, large masses or rapid tumor progression [81]. If the above treatments fail, new targeted drugs may be considered. The BTK inhibitor, ibrutinib, provides a chemotherapy-free treatment alternative for patients diagnosed with gastric MALT lymphoma. Remarkably, single-agent ibrutinib therapy has shown durable responses and a favorable benefit-risk profile in patients with gastric MALT lymphoma who have received prior treatment [70]. The PI3K inhibitor copanlisib has demonstrated significant efficacy and a manageable safety profile in patients with relapsed/refractory gastric MALT lymphoma who have received intensive treatment, and may be a salvage treatment option for patients [71].
Mycosis fungoides
Pathogenesis
Cutaneous lymphoma most commonly originates from T-cells [82]. Cutaneous T-Cell Lymphoma (CTCL) is broadly classified as a type of PTCL [83]. Mycosis fungoides (MF) is the predominant form of PTCL, constituting approximately 60% of all CTCL cases and approximately 50% of primary cutaneous lymphomas [82]. A dominant feature of MF is the presence of UV signature mutations, which contribute to a high tumor mutational burden. It is believed that UV exposure plays a role in the malignant transformation of skin-resident T-cells [84]. Besides, MF exhibits a complex genomic landscape characterized by frequent mutations in various genes involved in different cellular processes. These include genes associated with TCR signaling (PLCG1, CARD11, CD28, RLTPR), epigenetic regulation (TET2, DNMT3A, ARID1A/B), DNA damage response (TP53, POT1, ATM, BRCA1/2), and cell cycle control (CDKN2A/B, TP53) [85]. Moreover, aberrant activation of the NF-kB pathway is commonly observed in MF, primarily due to mutations in genes such as TNFRSF1B, NFKB2, PRKCB, and TNFAIP3 [86]. This activation leads to increased cell proliferation and survival. Furthermore, the JAK-STAT pathway is frequently dysregulated, with copy number gains in STAT3/STAT5B [85]. This dysregulation affects T-cell proliferation, differentiation, and gene regulation. Additionally, disruption of the PI3K/AKT/mTOR pathway, caused by mutations in PIK3CA, RHOA, and VAV1, further impacts T-cell metabolism, growth, and proliferation [27].
Epigenetic changes, including DNA methylation and histone modification, result in the dysregulation of gene expression in MF [87]. Subclonal evolution and intra-tumor heterogeneity are key aspects of MF pathogenesis [88]. These factors contribute to the diversity and complexity of the disease.
Diagnosis
Early patch/plaque stage MF can clinically mimic benign inflammatory dermatoses such as eczema or psoriasis, which initially presents a diagnostic challenge [89]. However, histopathology in early MF reveals a superficial perivascular and epidermotropic lymphocytic infiltrate. Immunophenotyping further demonstrates the presence of CD4 + small/medium pleomorphic T-cells [89]. To aid in the differentiation of early MF from its mimics, genomic profiling and the identification of mutations in genes such as TET2, DNMT3A, and TP53 can be utilized [85]. These molecular markers provide valuable insights for accurate diagnosis and management of the disease.
As MF progresses to advanced stages, the atypical CD4 + cerebriform lymphocytes become more prominent. In the tumor stage of MF, sheets of atypical lymphocytes can be observed. Additionally, Sezary syndrome, the leukemic variant of MF, is characterized by the presence of clonal circulating Sezary cells [89, 90].
Treatments
Early-stage MF can be managed using skin-directed therapies, such as topical steroids and phototherapy (UVA/UVB, PUVA). In cases of refractory disease, systemic retinoids or interferons may be employed [85]. For localized plaques and tumors, radiation therapy has proven effective but relapses frequently occur after a few months, and maintenance therapy is mandatory [91].
Conventional chemotherapy, like CHOP (cyclophosphamide, doxorubicin, vincristine, prednisone), yields poor outcomes in advanced MF [92]. However, promising results have been seen in relapsed/refractory cases of MF with the use of novel targeted therapies. These include JAK inhibitors, proteasome inhibitors, HDAC inhibitors, anti-CCR4 antibody, and PD-1/PD-L1 inhibitors [85]. As MF is a complex and chronic disease, it requires a multidisciplinary approach for effective treatment based on disease stage.
Natural killer T-cell lymphoma (nasal type)
Pathogenesis
NKTCL-NT is characterized by the malignant proliferation of CD56 + and cytoCD3 + lymphocytes and is known for its aggressive clinical course. This type of lymphoma is more commonly observed in Asian and Latin American populations [93, 94]. The most common sites of occurrence for NKTCL-NT are the nasal cavity, nasopharynx, and palate, followed by the oropharynx, hypopharynx, and tonsils [95].
The pathogenesis of NKTCL-NT involves Epstein-Barr virus (EBV) infection, which act as predisposing risk factors for the disease [96]. In EBV-infected NK/T cells, expression of latent membrane protein 1 (LMP1) and LMP2A is observed. LMP1, which mimics CD40, continuously activates AKT, STAT, JNK, MAPK, and NF-κB pathways. This activation inhibits apoptosis, promotes cell cycle progression, and modulates the immune system. Moreover, LMP1 can induce genomic instability by upregulating activation-induced cytidine deaminase. Genomic instability triggered by EBV infection further leads to somatic mutations in oncogenes and tumor suppressor genes, contributing to the development of EBV-associated NK and T-cell lymphomas [97]. On the other hand, LMP2A mimics the B cell receptor, leading to sustained activation of AKT, Syk, β-catenin, and protein kinase C. Consequently, this sustained activation promotes cell proliferation while inhibiting differentiation. Collectively, these mechanisms contribute to the pathogenesis of EBV-associated NK/T cell lymphoma [97].
The JAK/STAT pathway also plays a significant role for the development of NKTCL-NT. Mutations in the STAT3 gene are commonly observed in NKTCL-NT [98]. Activation of STAT3 is significantly correlated with the expression of programmed cell death-ligand 1 (PD-L1), suggesting that STAT3 activation leads to increased PD-L1 expression, promoting immune evasion by the tumor [99]. These findings suggest that immunotherapy targeting the programmed cell death 1 (PD-1)/PD-L1 checkpoint holds promise as a novel therapeutic option. In addition to the JAK/STAT pathway, other potential therapeutic targets in NKTCL-NT include Aurora kinase, MYC, NF-κB, FOXO3, deletion of chromosome 6q21-25, and promoter hypermethylation [100].
Diagnosis
Common primary symptoms of NKTCL-NT include nasal obstruction, nasal discharge, and nasal bleeding caused by nasal masses [95]. The occurrence of B symptoms is important in assessing NKT [95]. In the pre-treatment evaluation of NKTCL-NT, routine physical examinations, blood tests, biochemical examinations, enhanced whole-body CT scans, enhanced MRI, and endoscopy can be utilized. PET-CT is useful for staging, as lymphomas are known to have high avidity for 18-fluorodeoxyglucose [100]. Additionally, quantification of circulating EBV DNA serves as an accurate biomarker for assessing tumor load [100]. The typical immunophenotype of NKTCL-NT is determined based on pathological histology and immunohistochemistry. It is characterized by the absence of CD20, presence of CD3, lack of CD5, expression of CD56, high Ki-67 proliferation index, and increased levels of cytotoxic molecules such as granzyme B, perforin, and TIA-1 [100].
Treatments
Stage I NKTCL-NT patients without risk factors (age < 60 years, ECOG score 0–1, normal LDH, no extensive local invasion) can achieve favorable outcomes with radiotherapy alone [101]. On the other hand, stage I patients with risk factors and stage II patients are typically treated with a combination of radiotherapy and chemotherapy as the standard of care [102]. In stages I-II, the success of early NKTCL-NT treatment depends on the radiotherapy field and dose, which are closely associated with local control rates and prognosis [102].
L-menthanate-based chemotherapy regimens have shown the highest effectiveness in systemic treatment for NKTCL-NT [103]. One of these regimens is the SMILE regimen (dexamethasone, methotrexate, ifosfamide, L-asparaginase, and etoposide), which has demonstrated significant efficacy in primary stage III/IV and refractory relapsed cases [104]. Despite the improved response rates with L-menthanate-based chemotherapy, relapse still occurs in approximately 50% of patients with disseminated disease [100]. Targeted therapy, immunotherapy or transplantation may be options for patients with advanced, and relapsed/refractory NKTCL-NT.
The anti-PD-1 inhibitor sintilimab has shown unique efficacy in refractory relapsed NKTCL-NT, with preliminary results indicating an overall response rate of 67.9%, a complete response rate of 7.1%, and a 1-year overall survival (OS) rate of 82.1% [53]. Preliminary results from small-sample studies suggest that pembrolizumab may also have good efficacy [105]. Additionally, a phase II study has demonstrated the effectiveness of the histone deacetylase inhibitor chidamide in some patients, making it a potential option for those with refractory relapses [106].
Conventional chemotherapy alone has poor prognosis for relapsed/refractory NKTCL-NT. Although the value of ASCT remains controversial, several retrospective studies have shown that advanced or sensitive relapsed patients can benefit from ASCT after achieving high-quality remission [107,108,109]. Allogeneic transplantation is currently being explored due to its associated treatment-related risks but may be considered for refractory patients who have relapsed after autologous transplantation [109].
Primary central nervous system lymphoma
Pathogenesis
PCNSL is a highly aggressive, rare form of hematolymphoid tumor that occurs in the CNS, recognized as a primary large B-cell lymphoma of immune-privileged sites by the 5th edition of the World Health Organization Classification of Hematolymphoid Tumors [110,111,112]. PCNSL occur mostly among patients aged between 50 to70 and the median age at diagnosis is 65 [113]. The incidence of PCNSL has steadily increased over the past two decades, with an annual incidence rate of 0.4–0.5 per 100,000 [114,115,116,117]. The prognosis for PCNSL is poor, with a median survival of approximately 26 months [118] and the 5-year and 10-year survival rates of 35.2% and 27.5%, respectively [119].
Pathologically, more than 95% of PCNSL cases are diffuse large B cell lymphoma [120, 121]. Gene expression analysis confirmed that non-germinal center B-cell (GCB) is the most common phenotype in PCNSL patients [121,122,123,124]. PCNSL cases often carry mutations that lead to activation of the NF-κB pathway, such as activating mutations in MYD88, CDKN2A, TNFAIP3 and CD79B, suggesting that activation of the NF-κB pathway is a key driver of lymphangiogenesis in PCNSL[123, 125,126,127,128,129,130,131,132,133,134,135,136]. Based on the co-occurrence of the MYD88L265P and CD79B mutations, PCNSL is genetically of the MCD/C5 subtype [123, 125,126,127,128,129,130,131,132,133,134]. Common genomic and transcriptional hallmarks of PCNSL also include numerous BCR pathway related gene mutations [137,138,139,140,141,142,143], TLR pathway related gene mutations[135, 138, 139, 141,142,143,144,145], chromosomal translocations [146,147,148,149], aberrant somatic hypermutation [146, 150, 151].
Diagnosis
Patients with PCNSL typically emerge within weeks with neurological symptoms, such as focal neurological impairments (56–70%), altered mental state and behavior (32–43%), signs of raised intracranial pressure (headache, nausea, vomiting, optic papilledema; 32–33%), and seizures (11–14%) [152, 153]. On medical imaging, PCNSL usually appears as a uniformly enhancing mass, most commonly as a single brain lesion (66%), with a supratentorial position (87%) and frontoparietal lobe involvement (39%). Less frequently implicated are the eyes (15–25%), CSF (7–42%), and spinal cord (15–25%) [152]. To systematically assess the extent of disease involvement, the International PCNSL Collaborative Group suggests baseline staging, which includes MRI of the brain and spine, ophthalmologic evaluation, and CSF analysis [5]. In addition, a PET/CT and a bone marrow biopsy should be performed to assess whether PCNSL involves the non-central nervous system. The primary method for diagnosing PCNSL is a stereotactic biopsy. If there is a lot of damage to the eye or there are tumor cells in the CSF, a vitrectomy or CSF cytology may help confirm the diagnosis [152].
Treatments
High-dose methotrexate (HD-MTX) is the basis for the treatment of PCNSL [154,155,156,157,158,159,160,161,162,163]. Current major controversies in the treatment of PCNSL include the value and timing of surgery, the optimum chemotherapy regimen, the application of whole brain radiotherapy (WBRT), and the requirement for intrathecal chemotherapy [152]. Due to the high surgical risk posed by the broad and diffuse infiltrative growth of PCNSL, stereotactic biopsy is often employed to confirm the diagnosis. Surgical resection may also increase the risk of irreversible neurological damage [154].
Since the early 1980s, WBRT has been utilized to treat newly diagnosed PCNSL. When combined with HD-MTX, WBRT improved chemotherapeutic response and prolonged PCNSL survival [164,165,166,167,168]. Nonetheless, neurotoxicity has emerged as a significant factor influencing the quality of patient survival [169, 170]. Patients who received WBRT had considerably longer progression-free survival (PFS) than those who did not, but there was no significant improvement in the overall survival (OS) [169]. Clinical specialists are incredibly cautious when administering WBRT to PCNSL patients, especially to the elderlies, owing to the treatment's poor survival and significant neurotoxicity [169]. More alternative therapeutic strategies, including reduced-dose WBRT and local irradiation to the lesion to decrease neurotoxicity, are being evaluated in clinical trials in patients with PCNSL. Rituximab, a monoclonal antibody against B-cell surface antigen CD20, has been shown to enhance the clinical outcomes of PCNSL patients significantly [131, 163, 171,172,173,174,175,176,177]. Rituximab is currently used as an induction regimen in PCNSL with common regimens such as R-MVP (rituximab, methotrexate, procarbazine, and vincristine), R-MT (rituximab, HD-MTX, and temozolomide), Matrix (HD-MTX, cytarabine, thiotepa, and rituximab), or R-MVBP (rituximab, methotrexate, etoposide, carmustine, dexamethasone). Choosing the most appropriate chemotherapy regimen for PCNSL patients is a pressing challenge in clinical work. Lastly, there is no agreement on whether chemotherapy should be applied intracerebroventricularly. Even though intrathecal chemotherapeutic agents may prolong exposure to cytotoxic drugs in the CSF, they can also increase neurotoxicity [178].
Several novel treatments have shown efficacy and overall good tolerance in PCNSL patients, such as ASCT [179,180,181,182,183,184,185,186,187,188], BTK inhibitors [56, 189,190,191,192,193,194,195,196,197,198] and chimeric antigen receptor T-cells (CAR-T) [199,200,201].
Prognostic markers for PCNSL
In the past few decades, the prognosis of PCNSL has significantly improved due to the widespread use of HD-MTX chemotherapy and consolidation therapy. However, relapse remains common, with a 5-year survival rate of only 30% to 40% [114, 154]. Currently, common prognostic markers for PCNSL include basic characteristics, subtypes, imaging findings, prognosis scoring systems, clinical laboratory results, and biomolecules.
Utilization of basic patient characteristics as prognostic markers
Basic characteristics of PCNSL patients
According to a study comprising 466 PCNSL patients from 62 Japanese medical institutions, age > 60 years and the Eastern Cooperative Oncology Group Performance Status (ECOG PS) score > 2 were found strongly related to poor prognosis in PCNSL patients [202]. In a second study, Niparuck et al. additionally confirmed that ECOG PS score > 1 may function as an independent predictor of OS in multivariate analysis [203]. Furthermore, type B symptoms, multifocal lesions, meningeal spread, and higher lactate dehydrogenase (LDH) levels were linked to a worse prognosis [202].
Tumor localization
Patients with PCNSL have bad undesirable prognosis if the tumors are located in the deep brain, including the periventricular zone, basal ganglia, corpus callosum, brainstem and/or cerebellum [204,205,206,207,208]. Multivariate analysis of 101 newly diagnosed patients with PCNSL showed that deep brain lesions were an independent risk factor for PFS [204]. Another retrospective analysis of the clinical data of 89 patients with intracranial PCNSL by Ouyang et al. in 2020 showed that deep structural invasion was the independent risk factor for intracranial PCNSL [205]. Furthermore, patients with deep brain involvement have a higher risk of mortality in the first few months after diagnosis [208].
Mini-mental state examination
Mini-Mental State Examination (MMSE) is a tool for screening neurocognitive disorders [209,210,211,212]. In low-grade and high-grade gliomas, the MMSE score was an independent predictor of PFS and OS [213, 214]. A multicenter, phase III, and randomized trial examined the predictive value of the MMSE in 199 patients with PCNSL. All study subjects were adults with an ECOG PS score of 0 to 3, normal immune function, and CD20 positivity. One hundred and fifty-three patients out of 199 had MMSE scores at baseline. The MMSE score functioned as an independent predictor for OS and PFS in multivariate analysis. To summarize, the MMSE score is not only helpful in assessing the prognosis of patients with PCNSL, but it also straightforward and easy to use, making it useful in clinical practice [215].
Utilization of PCNSL cell of origin-based subtypes as prognostic markers
The classical PCNSL subtype by immunohistochemistry is based on the Hans algorithm, which is sorted by CD10, Bcl-6, and MUM-1 expression. Double expressor lymphoma has been utilized to classify PCNSL subtypes in recent years.
Figure 2 displays the classification criteria for the two subtypes of PCNSL.
Hans algorithm
DLBLC can be classified as GCB and non-GCB subtype according to Hans algorithm. The GCB subtype is associated with better prognosis in DLBCL [114]. Non-GCB was the most common phenotype in PCNSL patients, accounting for 65.7–96.3% of cases [121, 123, 130, 203, 216,217,218,219]. Besides, PCNSL was more commonly categorized in the non-GCB subgroup than DLBCL of peripheral nodal origin (p = 0.020; 78% vs. 62%), which may be primarily attributable to the increased nuclear MUM-1, also known as IRF-4, expression in PCNSL [220].
Hans algorithm may assist in determining the prognosis of PCNSL patients. In 2017, a study analyzed clinical, neuroimaging, and immunohistochemistry data from 41 PCNSL patients, who mostly received methotrexate-based chemotherapy-radiotherapy, to determine the impact of potential prognostic markers on clinical outcomes and the linkage between these markers. The GCB subtype was associated with a trend toward improved survival. However, neither OS nor PFS were statistically significant (p = 0.139 and p = 0.167, respectively) [218]. Another study included 43 patients with PCNSL, all receiving HD-MTX-based regimens, WBRT, or both. The OS of PCNSL was favorably linked with the GCB subtype [203]. Besides, a study investigated specimens and clinical data from 24 patients with biopsy-proven PCNSL and found that after a median follow-up of 15 months, only 39% of patients with non-GCB type PCNSL were alive, whereas all GCB type patients were alive. The median survival time for non-GCB patients was 11 months, but all GCB patients were still alive after a median follow-up period of 22 months [221]. Mechanistically, aberrant expression of BCL2 [203] or phosphorylation of the STAT3 protein [222] may contribute to the poor prognosis of PCNSL patients with non-GCB subtypes.
Although some investigations have shown no significant survival differences between the two categories of GCB and non-GCB [216, 219, 223], current studies tend to suggest that the prognosis for PCNSL patients with the GCB subtype of DLBCL is favorable.
Double expressor lymphoma
The identification of concurrent MYC and BCL2 (or BCL6) deregulation, whether at a genomic or protein level, has opened a new era of investigation within the most common subtype of PCNSL. Double-hit lymphoma (DHL), defined as a dual rearrangement of MYC and BCL2 and/or BCL6 genes [224,225,226,227]. Double-expressor lymphoma (DEL), defined as overexpression of c-MYC and BCL2 proteins not related to underlying chromosomal rearrangements [224, 228,229,230,231]. Both DHL and DEL are associated with a more aggressive clinical course and a worse prognosis for DLBCL patients [232]. Compared to DHL, DEL is more common in patients with PCNSL[130, 233, 234]. Therefore, we focused on the impact of DEL on the prognosis of PCNSL patients.
In a cohort of 48 individuals with newly diagnosed PCNSL, Hatzl S et al. followed 48 patients with newly diagnosed PCNSL for a median of 6.2 year. PCNSL patients with DEL characteristics had a 5-year risk of progression and/or death that was 13 times greater than those without DEL characteristics. Moreover, adding DEL in the International Prognostic Index (IPI) increases the model's prediction accuracy [235]. In 2022, a retrospective analysis was conducted on 82 pathologically proven, CD20-positive, PCNSL patients aged 71 or older who received therapeutic intervention in Japan. DEL was present in 43/82 (52.4%) cases. Multivariate analysis of the median OS revealed that DEL was the pathogenic risk factor [hazard ratio (HR) = 3.163, p = 0.004] [236]. A meta-analysis also confirmed that DEL was significantly associated with short median OS (HR = 1.23, p = 0.001) [237].
Imaging data as a prognostic indicator for PCNSL
Temporalis muscle thickness and L3 lumbar skeletal muscle index
Two muscle mass markers, temporalis muscle thickness (TMT) and L3 lumbar-skeletal muscle index (L3-SMI), were revealed to be independent predictors of PCNSL outcome. TMT is measured by MRI, which was found to be an independent predictor of OS in a study of 128 patients with primary PCNSL who had cranial MRI data [238]. In another study, 43 PCNSL patients who received first-line HD-MTX-based chemotherapy underwent brain MRI, and whole-body CT scans within 30 days of beginning treatment. Patients with low TMT levels had significantly worse PFS (HR = 4.40, p = 0.003) and OS (HR = 4.93, p = 0.002) than those with high TMT values [239].
The L3-SMI was calculated by first measuring the surface area of the abdominal and paraspinal muscles contained in the axial profile acquired at the third lumbar vertebra and then dividing the surface area by the square of the patient's height. According to the COX multivariate analysis in the preceding study [239], patients with low L3-SMI values had significantly shorter PFS (HR = 4.40, p = 0.003) and OS (HR = 3.16, p = 0.034) than those with high L3-SMI values.
Apparent diffusion coefficient
There are signs that a higher tumor cell density in diagnostic samples of PCNSL may have important prognostic effects. Because cellular density is negatively correlated with apparent diffusion coefficient (ADC) measurements on diffusion-weighted MRI (DWI), ADC values may predict the clinical prognosis of PCNSL patients [240]. The results suggest that lower ADC is associated with shorter PFS [240,241,242] or OS [240, 241, 243].
ADC values also correlated with the efficacy of HD-MTX-based chemotherapy regimens. A retrospective study of 28 patients treated with HD-MTX-based chemotherapy shows that there was a substantial between complete response (CR) and non-CR in terms of ADCmean and ADC5% percent. In addition, ADC5% percent beat ADCmean, as the area under the ROC curve (AUC) was greater for ADC5% compared to ADCmean (0.983 vs. 0.822) [242].
In summary, ADC values predicts PFS, OS, and the efficacy of HD-MTX in PCNSL patients.
Fluorodeoxyglucose-PET
Due to the high density of PCNSL tumor cells, quick glucose metabolism and high FDG content in the tumor, PCNSL demonstrates significant FDG uptake and can be diagnosed with an excessive degree of sensitivity using FDG-PET [244, 245]. FDG-PET can differentiate PCNSL from other forms of brain cancer [246,247,248,249]. In addition, FDG-PET may be more sensitive than conventional physical staging in the diagnosis of PCNSL and may detect the presence of additional concomitant systemic disorders [245, 250, 251]. Thus, FDG-PET is a non-invasive approach that may give verified prospective prognostic information for patients with PCNSL.
Kawai et al. performed FDG-PET in 17 patients with newly diagnosed PCNSL before treatment. FDG uptake was assessed by showing the standardized uptake value (SUV) of the tumor, showing the maximum uptake (SUVmax). This study showed that patients in the low and moderate uptake group (SUVmax < 12) had significantly better OS and PFS than those in the high uptake group (SUVmax ≥ 12), and therefore pretreatment FDG uptake could be used as a prognostic indicator for PCNSL [252]. Of note, Tateishi et al. found that NF-kB pathway activated RelA/p65-hexokinase 2, a rate limiting enzyme for glycolytic pathway [125]. Since most PCNSL harbors mutations in the MYD88 and CD79B, an upstream gene of the NF-kB canonical pathway, these mutations may contribute high uptake of FDG in PCNSL.
Prognosis scoring systems
For decades, five prognostic indexes have been proposed to stratify the clinical evolution of PCNSL (Fig. 3). Table 2 displays the detailed variables, hazard stratification, cancer types applied for the first time and disadvantages for these five prognosic scoring systems.
International prognostic index
The IPI is a broadly acknowledged prognostic score that may be used to differentiate between various risk categories of patients with DLBCL [253]. Twenty-five immunocompetent adult patients with PCNSL were treated in an early experiment with five cycles of HD-MTX-based chemotherapy followed by cerebral irradiation. The 2-year OS was 0% for patients > 60 years old with an IPI of 3 or more, compared to 88% for patients ≤ 60 years old with an IPI of 4 or less. The prognostic value of IPI in PCNSL was proven in this study [254].
International extranodal lymphoma study group score
In 2003 Ferreri et al. proposed the International Extranodal Lymphoma Study Group (IELSG), a scoring system based on clinical data of 378 PCNSL patients from 23 cancer centers in 5 countries from 1980 to 1999. The mean follow-up period was 24 months. It was found that age > 60 years, ECOG PS score > 1, elevated LDH levels, elevated CSF protein concentrations, and deep brain involvement could be independent prognostic markers for PCNSL. Based on the above findings, 105 evaluable patients were analyzed, and an IELSG prognostic model was developed, classifying adverse prognostic markers of 0–1, 2–3, and 4–5 as low, intermediate, and high-risk groups with 2-year OS rates of 80%, 48%, and 15%, respectively [206].
The prognosis model's accuracy can be increased by using the IELSG score in combination with additional prognostic parameters. A stronger predictive relevance can be seen, for instance, when the IELSG score is paired with the expression of programmed cell death ligand-1 (PD-1) on tumor-associated macrophages (IELSG-M). For OS, the areas under the receiver operating characteristic curves of IELSG-M were 0.844, which was higher than the IELSG model (0.580) [255].
Nottingham/Barcelona prediction score
The Nottingham/Barcelona prediction score includes three adverse prognostic variables, each with a value of 1. OS was negatively correlated with the Nottingham/Barcelona prediction score. The median survival for the 77 PCNSL patients included in the study was 55, 41, 32, and 1 month, with scores of 0, 1, 2, and 3, respectively [256].
Memorial Sloan-Kettering cancer center score
Age and karnofsky performance score (KPS) were the only two variables included in the Memorial Sloan-Kettering Cancer Center score (MSKCC score), and they were used to stratify participants into low-, intermediate-, and high-risk groups. The OS in PCNSL patients was negatively correlated with the MSKCC prognostic model score [207, 257, 258]. The largest study had 338 consecutive individuals with newly diagnosed PCNSL. The median OS for the low-, intermediate- and high-risk groups were 8.5, 3.2, and 1.1 years (p < 0.001), respectively. The median failure-free survival for the low-, intermediate- and high-risk groups were 2, 1.8, and 0.6 years (p < 0.001) [257]. Notably, one study found no significant difference in OS between the low- and intermediate-risk groups based on the MSKCC score [258]. Additional prognostic variables, such as lactate dehydrogenase/lymphocyte ratio (LLR) [258] and hemoglobin (Hb) [259], should be added to the MSKCC model to improve it further.
Taipei score
The researchers discovered that the IELSG, Nottingham/Barcelona, and MSKCC models are not sufficiently satisfactory for differentiating PFS or OS in patients with PCNSL. In order to construct a more accurate prognostic model, the researchers recruited 101 newly diagnosed PCNSL patients. Age ≥ 80 years, ECOG PS score ≥ 2, and deep brain lesions were identified as independent adverse prognostic markers for PFS by multivariate analysis. Researchers scored one point for each adverse prognostic factor and developed a new predictive model, the Taipei score, with four different risk categories (scores 0–3). In the training cohort, the Taipei score distinguished between PFS and OS significantly, and the score was verified in an external validation cohort. The Taipei score is therefore expected to provide the classification of disease risk for PCNSL and improve clinical decision-making [204].
Utilization of routine hematological indicators as prognostic indicators
Pre-treatment hematology is a routine test for all patients and is a convenient way to predict the prognosis of PCNSL. Hematologic indicators also can be used in combination with prognosis scoring systems to improve predicted accuracy. Table 3 displays the findings of studies utilizing conventional hematological clinical markers as prognostic indicators.
Lymphocyte count
Lymphocyte count (ALC) has predictive relevance in non-Hodgkin’s lymphoma [260, 263,264,265]. In 2016, Korean researchers first discovered that pretreatment ALC also could be an independent prognostic marker in PCNSL patients. They analyzed 81 PCNSL patients treated with HD-MTX and developed a new predictive model based on ECOG PS score > 1, age > 50 years, and the existence of decreased ALC, assigning 1 point to each factor and categorizing patients into three risk groups: low (0–1), intermediate (2), and high (3). Patients in the low, moderate, and high-risk categories had 5-year survival rates of 74.3%, 21.7%, and 12.5%, respectively [260]. Because of the convenience and low cost of detecting ALC, this model could be utilized as an objective and reliable prognostic tool for PCNSL. Notably, the predictive importance of ALC and this model needs be confirmed in a larger number of samples.
Neutrophil/lymphocyte ratio
Tumor cells release cytokines and chemokines to attract immunological and inflammatory cells, which stimulate tumor growth and survival [266,267,268,269,270,271,272,273,274,275,276]. A high neutrophil count may be a marker of inflammation, while a low lymphocyte count may indicate a lack of host immunity [277]. Hence, a high neutrophil/lymphocyte ratio (NLR) before therapy may therefore be one of the negative prognostic variables. Recently, high pre-treatment NLR has been proven to be an independent marker of poor prognosis in DLBCL [278, 279].
For PCNSL, high NLR was an independent prognostic factor [258, 261, 262]. High NLR was significantly associated with a worse PFS [261] and OS [258, 261] for PCNSLs by univariate analysis. Due to the strong lympho-toxic effects of steroids, the use of steroids prior to chemotherapy in PCNSL patients may affect NLR [280]. In the recent study, 75 individuals who had received chemoimmunotherapy were included. The study calculated NLR at three-time points: baseline (pre-steroid), pre-chemoimmunotherapy (post-steroid) and post-chemoimmunotherapy. The results suggest that OS was longer with higher pre-chemoimmunotherapy (post-steroid) NLR (dichotomized at NLR ≥ 4.0, HR = 0.42, 95% CI: 0.21–0.83, p = 0.01) [280]. It is hypothesized that steroid therapy, when combined with NLR, can successfully calibrate the PCNSL prognostic model and increase the accuracy of NLR in determining patient prognosis.
Lactate dehydrogenase/lymphocyte ratio
The lactate dehydrogenase/lymphocyte ratio (LLR) has been shown to be an independent prognostic factor in patients with extranodal natural killer/T-cell lymphoma [281], DLBCL [282, 283] and metastatic renal cell carcinoma [284]. Clinical data from 248 patients with PCNSL diagnosed at six cancer facilities in 4 countries were analyzed from 2004 to 2019 to see if LLR could be used as a promising predictive model for PCNSL. OS was selected as the study's endpoint. According to univariate analysis, LLR values greater than 166.8 were significantly related to a poorer OS. LLR was also shown to be an independent prognostic parameter for poorer OS by multivariate analysis. Notably, there was no significant difference in OS between the low- and intermediate-risk groups according to the MSKCC score; however, LLR could be an independent prognostic indicator for these patients [258].
Hemoglobin
Anemic individuals account for 30% to 90% of cancer patients [285,286,287,288]; nevertheless, Hb measurement is impacted by potentially confounding factors. The most common confounding variable is the use of corticosteroids by a portion of PCNSL patients, which may influence hemoglobin levels. Additionally, patients with tumors frequently have one or more concurrent anemia-causing causes, such as inflammatory anemia, chronic illness anemia, or bleeding disorders. Hb was an independent prognostic factor for PCNSLs (HR = 3.94, p = 0.013) [262]. In 2019, a retrospective study of 182 newly diagnosed PCNSL patients from a single medical center indicated that anemia was significantly associated with poor OS. Notably, combining Hb enhances MSKCC's accuracy in predicting PCNSL outcomes [259].
Systemic immune inflammatory index, lymphocyte/monocyte ratio and total bilirubin
There is growing evidence that cancer-related inflammation can promote the growth, invasion, and metastasis of cancer cells [289,290,291,292,293,294,295,296,297,298,299]. As a component of the innate immune system, neutrophils are an indicator of ongoing systemic inflammation. Additionally, neutrophils may contribute to the suppression of lymphocyte function, promote tumor immune escape and facilitate metastasis [300]. Nevertheless, the predictive significance of peripheral blood markers indicative of systemic inflammation and nutritional status in patients with PCNSL is uncertain. Systemic immune inflammatory index (SII) is an index of systemic inflammatory response calculated from platelet count × neutrophil count/lymphocyte count. A retrospective study analyzed 60 patients with HD-MTX-based standard chemotherapy PCNSL diagnosed from 2011 to 2020. Lymphocyte/monocyte ratio (LMR) (HR = 24.040, p = 0.019), SII (HR = 11.174, p = 0.002) and total bilirubin (TBIL) (HR = 5.245, p = 0.002) were independently associated with OS in this multivariate analysis. The C-index of the MSKCC score increased from 0.57 to 0.72 when SII and TBIL were added, indicating that the addition of SII and TBIL improved the ability of the MSKCC score to predict survival in PCNSL patients treated with the HD-MTX regimen [262].
Biomolecules as prognostic indicators in PCNSL
miRNAs
MicroRNAs (miRNAs) are involved in every biological process relevant to cancer, including cell proliferation, differentiation, death, and metabolism [289,290,291,292,293,294,295,296,297,298,299]. Importantly, the biogenesis and activation of miRNAs are faster with longer half-lives compared to mRNA and proteins, which may make miRNAs more suitable for earlier detection [301,302,303,304,305,306,307,308,309,310].
One study examined the levels of circulating miRNAs in PCNSL patients and found that miR-151a-5p and miR-151b could significantly differ short-term from long-term survival [311]. Mao et al. found that miR-21 was significantly elevated in the serum of PCNSL patients compared to other brain tumors and normal controls. Kaplan–Meier survival curves shown higher expression level of serum miR-21 was tightly associated with a poor prognosis in both test and validation cohorts [312]. In another trial assessing the efficacy of pemetrexed plus rituximab as second-line treatment, higher blood miR-21 levels indicated shorter survival, with a PFS of 5.7 months compared to 9.0 months when serum miR-21 levels were lower [313]. miR-30d, miR-93, miR-181b [314], miR-101, miR-548b, miR-554, and miR-1202 [315] have also been reported to be promising as useful prognostic markers for PCNSL. Eight hundred and forty-seven miRNAs expressed in 27 PCNSL specimens were analyzed using microRNA microarrays by Takashima et al. Multivariate analysis revealed that the combination consisting of miR-30d, miR-93 and miR-181b was an independent factor for poor OS in PCNSL [314]. In addition, Takashima et al. detected 847 miRNAs in 40 PCNSL patients using microRNA microarrays, containing 334 miRNAs associated with cancer immune-related genes (associated with regulation of type 1/2 T-helper (Th) cell status, T-reg cell status and immune checkpoints status, respectively), using four of these representative miRNAs (miR- 101, miR-548b, miR-554, and miR-1202) combined with patient clinical information to obtain a prediction formula, and patients in the low group had better OS [315].
snRNAs
Small nuclear RNAs (snRNAs) are a subtype of short-stranded non-coding RNA [316,317,318]. Existing research on the prognostic and diagnostic significance of snRNAs is still limited. Given that circulating U2 small ribonucleic acid fragments (RNU2-1f) serve as novel blood biomarkers for pancreatic, colorectal, and lung malignancies, the function of RNU2-1f in the CSF of PCNSL patients was investigated [319]. Researchers collected sequential CSF samples from nine PCNSL patients and then used real-time PCR to evaluate RNU2-1f levels. The results indicated that CSF RNU2-1f expression was positively linked with disease development based on serial measurements of RNU2-1f from nine patients with varying disease stages. In addition, CSF RNU2-1f levels appeared to correspond with MRI-measured tumor volume. The results presented above demonstrate that the level of RNU2-1f in CSF is a viable biomarker for determining the prognosis of PCNSL [319].
MYC
MYC (also called c-MYC in protein level) is one of the most prominent prognostic factors in PCNSL and can function at three levels: RNA, DNA, and protein. In a retrospective analysis, Gomes Candido Reis D et al. identified overexpression of MYC as a poor prognostic indicator of PCNSL [47]. RNA was isolated from 35 formalin-fixed and paraffin-embedded (FFPE) tissue samples. Following this, quantitative reverse transcription-PCR was performed for MYC. Relative gene expression of MYC ≥ 0.201 was linked with worse OS (HR = 6.117, p = 0.003) and worse PFS (HR = 3.960, p = 0.016). Another study found significant differences between the Kaplan–Meier curves in the mutant and wild-type groups, suggesting that somatic mutations in MYC (HR = 0.305, p = 0.0012) at the DNA level were associated with better overall survival (OS). These findings indicate that somatic mutations occurring specifically in the MYC are potentially important diagnostic and prognostic markers for PCNSL tumorigenesis and patient survival [320]. Overexpression of c-MYC [218, 235, 321] in protein level is also widely recognized to be associated with poor prognosis in PCNSL. To comprehensively assess the predictive role of c-MYC protein expression in PCNSL, Ge et al. conducted a meta-analysis [237]. Thirty-one studies involving 1739 patients were included in this meta-analysis. C-MYC expression was significantly associated with median OS and PFS. Subgroup analysis revealed that c-MYC protein positive remained a significant predictor of short median OS in studies with 45 participants, no WBRT, a quality scale score over 6, and a positivity threshold set at 40% stratum.
BCL2 and BCL6
The prognostic role of BCL2 and BCL6 in PCNSL remains controversial. Overexpression of BCL2 [235, 321], and/or BCL6 [218, 321] is generally believed to be associated with a poor prognosis in PCNSL. However, contradictory findings have been reported regarding the predictive value of BCL2 [322] and/or BCL6 [219, 322] in predicting survival in PCNSL patients.
The disparate outcomes of the research above may be attributable to the small sample sizes of the trials and the variety of patients' treatment regimens. The meta-analysis mentioned above also comprehensively assessed the predictive role of BCL2 and BCL6 protein expression in PCNSL [237]. BCL6 protein positivity is associated with a favorable prognosis. There was no significant correlation between BCL2 expression and OS or PFS, but BCL2 and c-MYC co-expression were significantly associated with short median OS. As most of these included papers are retrospective studies, the prognostic effect of BCL2 in PCNSL needs further validation.
CD79B
Recurrent mutations in CD79B are characteristic of PCNSL, and 69–83% of PCNSL patients were found to have recurrent CD79B mutations by sequencing [57, 58]. Recurrent CD79B mutations were found in 69–83% of PCNS L patients. The relationship between CD79B and PCNSL prognosis is not yet clear. According to Zhou Y et al., patients with lymphoma who harbored the CD79B mutation had significantly worse PFS than patients with wild-type CD79B [58]. Another study presented the opposite result. Another study with Hispanic PCNSL patients revealed the opposite findings, demonstrating that CD79B mutations were associated with improved 2-year PFS [323].
MYD88
MYD88L265P, is an important oncogene for lymphoma [324,325,326,327]. With the advancement of high-throughput molecular technologies, it has been found that mutations in the MYD88L265P gene are present in 55–88% of patients with PCNSL [132, 328,329,330,331]. Moreover, the protein expression of MYD88 was significantly elevated in PCNSL patients in comparison to individuals with lymphadenitis (70.18% vs. 15%) [58].
Hattori K et al. demonstrate for the first time that MYD88L265P mutation is independently associated with shorter OS and PFS in PCNSL [329]. MYD88L265P mutation is more prevalent in patients over 65 years old. The Kaplan–Meier analysis revealed that MYD88L265P mutation predicted shorter OS (11.5 months vs. 56.2 months, p < 0.04) in patients older than 65 years [330]. Besides, Zhou Y et al. investigated tissue samples from 57 PCNSL patients using immunohistochemistry and discovered that a high level of MYD88 expression was an independent predictor of OS (HR = 0.143, p = 0.004) [58]. PCNSL patients with high MYD88 expression had a shorter OS than those with low expression (8 months vs. 31 months, p = 2.0 × 10−6).
However, a study suggested that MYD88L265P mutation is a favorable prognostic factor for PCNSL. MYD88L265P mutation status was available in 41 PCNSL patients with non-GCB subtypes, 36 (88%) of whom were mutants. The MYD88L265P mutation was linked to better survival in the multivariable model (HR = 0.277; p = 0.023) [328].
ATP binding cassette subfamily B member 1
ATP Binding Cassette Subfamily B Member 1 (ABCB1), one of the key ABC transporters of the blood–brain barrier (BBB), can be classified into two genotypes with T (genotypes CT and TT) and without T (genotype CC) [332,333,334]. The rs1045642 is the most common of the ABCB1 gene polymorphisms [335]. It has been reported that the CC genotype of ABCB1 rs1045642 is related to MTX-induced mucositis [336] and poorer event-free survival (EFS) [337] in hematological tumors. Wu et al. conducted a prospective study of 91 patients with PCNSL enrolled at Huashan Hospital from 2006–2015. Multivariate analysis showed that ABCB1 rs1045642 was an independent risk factor for PFS and was associated with a higher risk of progression, suggesting that assessing the genetic variability of patients provides another possible method to assess the prognosis of PCNSL [335].
Ki-67
Ki-67 expression levels indicate the level of cell proliferation. Ki-67 (90% cutoff) was associated with shorter OS (p = 0.037) and PFS (p = 0.039) in a cohort of 89 PCNSL cases. However, in the multivariate analysis, Ki-67 failed to predict prognosis [322]. In another study that included 45 patients with PCNSL, Ki-67 index ≥ 90% was an independent predictor of poor OS prognosis in the entire cohort as well as in the non-GCB tumor subtype (Ki-67 index = 91.1%) [223].
p27
P27 is a cyclin-dependent kinase inhibitor that controls the progression of the cell cycle from G1 to S phase [338]. Kunishio et al. employed immunohistochemistry to examine p27 expression in 22 PCNSL patients. High p27 expression was found to be highly related to shorter OS, implying that p27 might be used to predict the prognosis of PCNSL patients [338].
Histone methylation abnormality
Numerous genetic alterations in cancer are associated with chromatin and epigenetics, particularly histone-modified proteins. Histone modifications have a crucial role in both normal cell function and malignancy. Common modifications of histones include methylation, acetylation, ubiquitination, and phosphorylation [339]. Histone modifications have a crucial role in malignancy. Researchers immunohistochemically stained FFPE samples from 87 PCNSL patients identified by pathology. Patients with H3K4me3 hypomethylation and H3K27me2 and H3K27me3 hypermethylation were more likely to relapse. In both univariate and multivariate studies, these three variables were statistically related with a short PFS and OS. It was shown that low methylation of H3K4me3 and high methylation levels of H3K27me2 and H3K27me3 may be linked to a poor prognosis in PCNSL patients [340].
PD-1, PD-L1, and PD-L2
Expression levels of PD-1, PD-L1 and PD-L2 on PCNSL tumor cells can be utilized to predict patient prognosis. Takashima Y et al. performed RNA sequencing on samples from 31 PCNSL patients and found that changes in the expression of PD-1 and PD-L2 transcripts enable prognostic prediction in PCNSL. High PD-1 (PDCD1-001: HR = 3.3, p = 0.012, PDCD1-002: HR = 9.3, p = 8.4E-05, and PDCD1-003: HR = 2.6, p = 0.032) and PD-L2 (PDCD1LG2: HR = 2.9, p = 0.018) gene expression was associated with a shorter OS [341]. Cho et al. analyzed the prognosis of 76 patients with PCNSL who received an HD-MTX-based chemotherapy regimen at the time of first diagnosis. The multivariate analysis revealed that high PD-1 expression (70 cells/high power field) was associated with a worse OS and a PFS [342]. Analysis of PD-L1 expression in serum and FFPE tissues of PCNSL patients revealed that the median level of serum PD-L1 was greater than that of healthy control patients; PD-L1 expression of positive tumor cells in FFPE tissues was positively correlated with serum PD-L1 level. Notably, the high serum PD-L1 group was more susceptible to recurrence than the low serum PD-L1 group [343].
The tumor microenvironment, in addition to tumor cells, influences PCNSL prognosis. Using immunohistochemistry techniques, Furuse et al. evaluated intratumoral and peritumoral tissues from 70 patients with PCNSL. It was discovered that a greater proportion of macrophages than tumor cells expressed PD-L1 and PD-L2. PD-L1 expression on macrophages was linked to biological factors (intratumoral macrophages: better KPS, better MSKCC score, and peritumoral macrophages: low proportion of LDH elevation) and a longer OS correlation [344]. Another study also confirmed that the increased number of PD-L1-expressing immune cells, like tumor-infiltrating lymphocytes and tumor-associated macrophages, is associated with better disease-free survival in PCNS-DLBCL [345].
Ku80
Ku80 is a DNA repair protein connected with radiosensitivity and plays a crucial role in multiple processes that protect against ionizing radiation. In a study reviewing 38 patients with PCNSL, Ku80 expression in tumor tissue was found to be present in most PCNSL tissues using immunohistochemistry. According to survival analysis, patients with high Ku80 expression had significantly shorter median survival times than patients with low Ku80 expression (p = 0.036). Intriguingly, although Ku80 was connected with radiosensitivity, it was not statistically significant when comparing the OS of patients treated with and without radiotherapy (p = 0.131). Consequently, Ku80 is anticipated to be a prognostic predictor for PCNSL [346]. Due to the small number of patients described in this study (n = 38), the conclusion that Ku80 cannot be used to predict radiotherapy efficacy requires further validation.
CD105
CD105 is a receptor for transforming growth factor (TGF)-beta1 and -beta3, and its interaction with TGF-beta receptors I and/or II modulates TGF- signaling [347,348,349,350,351,352,353]. Furthermore, CD105 is a proliferation-associated hypoxia-inducible protein that is overexpressed on proliferating endothelial cells engaged in tumor angiogenesis but is low or not expressed in normal tissues' vascular endothelial cells [349].
The current study investigated the link between CD105 expression and PCNSL prognosis using immunostaining for CD105. Intratumoral microvascular density (IMVD) was measured in the hotspots and interfaces at a magnification of × 200. When CD105 was utilized as an angiogenesis marker, the lower-IMVD group had a significantly greater survival rate than the higher-IMVD group. The IMVD was larger in the hotspots than in the interfaces in the group with CD105-immunostained vasculature. These findings revealed that PCNSL growth depended on angiogenesis and that IMVD, measured by an anti-CD105 monoclonal antibody, was a reliable prognostic marker in PCNSLs [354].
Glucose transporter protein type 1
The process of glucose metabolism is crucial in cancer development [355,356,357,358,359,360,361]. MTX resistance in PCNSL cells is possibly associated with altered aerobic glycolysis [362]. According to a Korean study, PCNSL patients expressed glucose transporter protein type 1 (GLUT1) in tumor tissues, and patients with > 20% GLUT1 positivity in lymphoma cells had shorter OS and more rapid disease progression [363]. GLUT-1 may affect the prognosis of PCNSL patients by having an impact on the mean value of fasting plasma glucose (FPG) levels. The percentage of GLUT1-positive cells was higher in patients with FPG ≥ 110 mg/dL (p = 0.015), while high mean value of FPG was a significant predictor for shorter survival (p = 0.036) [364]. The results of the current research suggest that the expression level of GLUT1 is associated with PCNSL prognosis.
PI3K/AKT/mTOR pathway-related proteins
Since the PI3K/AKT/mTOR pathway is aberrantly active in DLBCL and plays a role in the genesis and progression of DLBCL [365,366,367,368,369], researchers have also investigated its role in PCNSL. Zhang et al. found that the recurrence rate of PCNSL in the phospho-mTOR-positive group was 64.5%, which was substantially greater than in the negative group. The Kaplan–Meier survival analysis revealed shorter PFS in the phospho-mTOR and phospho-S6-positive groups, while PTEN loss was associated with a shorter OS. According to Cox regression analysis, phospho-mTOR expression was an independent predictor for shorter PFS. The results reveal that the PI3K/AKT/mTOR pathway is aberrantly active in PCNSL and linked with a poor prognosis, which may foreshadow the development of novel therapeutic targets and prognostic variables [365].
Interleukin-10
Interleukin-10 (IL-10) is a pleiotropic cytokine produced by T helper-2 cells, monocytes, macrophages, and B lymphocytes [370,371,372,373,374,375,376]. IL-10 not only has broad-spectrum anti-inflammatory effects but also promotes the expression of BCL-2 and protects malignant tumor cells from apoptosis [377]. Since IL-10 appears to activate STAT3, it contributes significantly to the development of PCNSL [378]. Increased IL-10 levels in CSF indicated poor KPS scores and reduced PFS or OS periods [377, 379, 380]. In a prospective study, CSF IL-10 levels were measured in 66 intracranial tumors, 26 of which were PCNSL and 40 of which were other brain tumors. The PCNSL levels were significantly higher than the other brain tumor levels. The level of IL-10 in the CSF was reduced in all patients after therapy but rose in most recurrence patients. Higher levels of IL-10 in CSF were linked to a shorter PFS [377]. The results suggest that IL-10 levels in the CSF may be a sensitive biomarker for differential diagnosis, early relapse monitoring, prognosis assessment, and evaluating the effectiveness of PCNSL. High level of IL-10 in CSF increases TAMs filtration in PCNSL, leading to shorter PFS (p = 0.04) [381].
Apart from the aforementioned biomolecules, some other biomolecules, such as PAX5 [320], FOXO1 [320] and Mismatch repair protein MSH2 [218], have also been found to be closely associated with the prognosis of PCNSL. Table 4 presents the outcomes of investigations utilizing biomolecules as PCNSL prognostic markers.
Challenges and future perspectives
Currently, multiple prognostic markers are applied to predict the prognosis of PCNSL patients (Fig. 4). Basic PCNSL patient characteristics, imaging, treatments and subtypes help determine PCNSL prognosis. However, the sensitivity, specificity, and survival benefit of the predictors are usually unsatisfactory for routine screening.
An overview of the prognostic factors currently utilized to predict PCNSL. Abbreviations: ABCB1, ATP Binding Cassette Subfamily B Member 1; ALC, Lymphocyte count; ECOG PS, The Eastern Cooperative Oncology Group Performance Status; GLUT, Glucose transporter protein type; H3K27, Histone H3 lysine 27; H3K4, Histone H3 lysine 4; Hb, Hemoglobin; IELSG, International Extranodal Lymphoma Study Group; IL-10, Interleukin-10; IPI, International Prognostic Index; LLR, Lactate dehydrogenase/lymphocyte ratio; LMR, Lymphocyte/monocyte ratio; miRNA, MicroRNA; MSKCC, Memorial Sloan-Kettering Cancer Center score; MYD88, Myeloid differentiation major response gene; NLR, Neutrophil/lymphocyte ratio; PD-1, Programmed cell death-1; PD-L1, Programmed cell death-ligand1; PD-L2, Programmed death-ligand 2; SII, Systemic immune inflammatory index; snRNA, Small nuclear RNA; TBIL, Total bilirubin
The prognosis scoring systems are commonly used in clinical practice, and therefore receive the most attention. For IPI scoring, the classification of PCNSL ‘clinical staging’ directly impacts on the patients’ scores. Some researchers classified PSNCL as grade I-II (tumors all located on the same side of the diaphragm), while other researchers classified PCNSL as grade IV (diffuse or disseminated involvement of one or more extra-lymphatic organs). This difference in classification may affect the accuracy of IPI scoring.
Nottingham/Barcelona prediction score, which is modified form of the IPI score, and the Taipei score are used less frequently. Therefore, the accuracy of assessing the prognosis of PCNSL using the above scoring systems needs large population validation.
Currently, the internationally recognized and more widely used score for assessing PCNSL prognosis in clinical practice are the MSKCC and the IELSG score. The MSKCC prognostic model has a selection bias due to the reason that the study population is usually from the same institution [257].
IELSG score sometimes cannot be performed in PCNSL patients due to the lack of CSF protein results. Patients with PCNSL show occupying intracranial lesions with perifocal edema, and are at risk of increased intracranial pressure and potential complications. Therefore, lumbar puncture is not always performed in routine clinical practice [207].
In addition, both the MSKCC and the IELSG score are based on retrospective studies, and the treatment regimens of most patients are based on HD-MTX. With the advances in the clinical management of PCNSL, such as the widespread use of MATRix protocols, these models may not always be applicable to today's PCNSL treatment paradigm.
In recent years, more prognostic studies are performed based on laboratory hematological tests. Clinically used hematological markers, such as ALC, LLR, NLR and Hb are cost-effective, easily accessible, and to some extent, can reflect patient treatment and prognosis. However, it should also be noted that they are not as sensitive and specific for PCNSL. These indicators are susceptible to tumor comorbidities and complications, such as anemia, cachexia, chronic inflammation, and organ insufficiency.
C-MYC and BCL2 are two of the most studied proteins as they are associated with the DEL subtype classification of PCNSL. The DEL subtype can not only predict the PCNSL prognosis alone, but can also be combined with the IPI score to improve the prediction accuracy. The significance of new prognostic markers (e.g., RNA, DNA and proteins) in assessing PCNSL prognosis is being investigated. The factors that currently have clear prognostic significance for PCNSL include MYC, PD-1, MyD88L265P mutation, ki67, PD-1, c-MYC and IL-10 in CSF. To date, the prognostic efficacy of most factors is controversial. The role of some key factors in predicting PCNSL prognosis is unclear, such as the proto-oncogene serine/threonine (Ser/Thr) protein kinase 1 (PIM1), a known target for somatic hypermutation mechanisms in PCNSL [150, 320, 383].
Since the presented prognostic biomarkers or models for PCNSL are still unsatisfactory; new effective prognostic biomarkers and/or models are required to assist clinicians in determining the clinical progression of PCNSL and achieving more accurate therapeutic stratification.
Firstly, combining traditional tests with existing prognostic models can improve the accuracy of PCNSL prognosis. For example, the MSKCC score combined with LLR can effectively improve the accuracy of prognostic assessment in low and intermediate-risk groups [258]. Secondly, new body fluid biopsy techniques (including circulating tumor DNA, circulating tumor cells, cell-free RNA, tumor cultured platelets and exosomes) should be considered to be included in PCNSL prognostic models. The potential utility of liquid biopsy for early detection and management of cancer has emerged as a promising alternative way over traditional tissue sampling methods [384]. Thirdly, some prognostic genes, including somatic mutations, copy number variants, fusion gene alterations, may have an impact on PCNSL prognosis. Taking MYD88 as an example, it can influence PCNSL prognosis through both aberrant expression and mutations. Future studies require subgroup analysis based on marker variants. Moreover, almost all current prognostic studies are retrospective. Prospective studies are needed to aid better stratification of PCNSL patients, and assessing the technical robustness and reproducibility of the proposed biomarkers by implementing stringent inclusion and exclusion criteria, so that patient inconsistency can be reduced. Besides, multicenter studies should be conducted through international collaborations. To improve the accuracy of study results, large-scale, forward-looking studies are needed. Finally, some novel factors have been found to express in specific PCNSL populations. For sample, N-linked oligosaccharides [385], PI3K/AKT/mTOR [362] pathway and oxidative stress [362] have been reported in relapsed or MTX-resistant PCNSL patients. PCNSL prognostic models should be developed in the future for EBV-positive, HIV-positive and rituximab populations, as well as for populations with alternative treatment methods (such as BTK inhibitors, proteasome inhibitor [386], and hematopoietic stem cell transplantation). However, due to low prevalence of PCNSL, multicenter, large-scale population and prospective studies of prognostic factors should require global collaboration.
With advances in testing technology and the development of large-scale, multicenter, prospective and international collaborative clinical studies, the technical challenges of testing PCNSL samples and the problem of biased patient data selection have been gradually overcome. New prognostic assessment models are expected to enter the clinics to assist clinicians in their decision-making.
Conclusion and prospect
In summary, the pathogenesis of extranodal lymphoma involves a variety of mechanisms, including genetic alterations, immune dysregulation and viral infection. Viral infections are an important causative factor in extranodal lymphoma, including HP, EBV, HBV, HCV and HIV [387]. The pathogenesis of extranodal lymphoma of B-cell, T-cell and NK-cell origin varies widely. The exact pathogenesis of extranodal lymphoma is still being explored and is thought to be a complex interplay of environmental and genetic factors.
Extranodal lymphoma differs from common diseases at the site of origin or secondary lymphoma involving that site, but its clinical presentation and imaging features are often nonspecific. Therefore, a pathological biopsy is required to confirm the diagnosis. The diagnostic process involves evaluating the location, pathological type, extent, stage, immunophenotype, molecular biology, and patient-related factors of the disease. Tissue biopsy and immunohistochemistry are most important in determining the specific subtype and cell origin. Staging and risk stratification are crucial for designing an appropriate treatment plan.
The treatment approach depends on the stage and subtype of the disease. For localized disease, radiotherapy or chemotherapy alone may be effective in some cases. However, for advanced or disseminated disease, a combination of radiotherapy and chemotherapy is typically recommended. Conventional chemotherapy alone has limited success in relapsed/refractory cases. ASCT after achieving remission can benefit selected patients, while allogeneic transplantation is being explored for refractory cases.
Individualised treatment based on pathogenesis is important in extranodal lymphoma. Clinical trials have relatively focused on inhibitors targeting the PI3K/Akt/mTOR, PD-1/PD-Ls, and BCR pathways, showing promising results in relapsed/refractory extranodal lymphoma. In addition to specific pathway inhibitors, pan-pathway inhibitors are also being extensively studied. For example, MS-553, a protein kinase C (PKC) inhibitor, can act on several classical signaling pathways, such as the PI3K/Akt/mTOR pathway, the MEK/ERK pathway, and the NF-κB pathway [388]. CTLA-4 inhibitors, DNA methyltransferase inhibitors, chimeric antigen receptor T-cell therapy are also being explored in relapsed/refractory lymphomas, and there is hope for future use in extranodal lymphomas as well [389].
In conclusion, a comprehensive approach combining radiotherapy, chemotherapy, targeted therapy, immunotherapy, and transplantation offers the best chance for successful management of extranodal lymphoma. Further research is needed to better understand the underlying mechanisms and optimize treatment strategies for this complex disease.
Availability of data and materials
Not applicable.
Abbreviations
- ABCB1:
-
ATP Binding Cassette Subfamily B Member 1
- ADC:
-
Apparent diffusion coefficient
- AKT:
-
Protein kinase B
- ALC:
-
Lymphocyte count
- AUC:
-
Area under the ROC curve
- ASCT:
-
Autologous stem-cell transplant
- BAFF:
-
B-cell activating factor
- BCR:
-
B-cell receptor
- BTK:
-
Bruton's tyrosine kinase
- CAR-T:
-
Chimeric antigen receptor T-cells
- CDK:
-
Cyclin-dependent kinase
- CNS:
-
Central nervous system
- CSF:
-
Cerebrospinal fluid
- CR:
-
Complete response
- C-index:
-
Harrell’s concordance index
- DEL:
-
Double expressor lymphoma
- DLBCL:
-
Diffuse large B-cell lymphoma
- DSS:
-
Disease-specific survival
- DWI:
-
Diffusion-weighted MRI
- EBV:
-
Epstein-Barr virus
- ECOG PS:
-
The Eastern Cooperative Oncology Group Performance Status
- EFS:
-
Event-free survival
- FDG:
-
Fluorodeoxyglucose
- FFPE:
-
Formalin-fixed and paraffin-embedded
- FPG:
-
Fasting plasma glucose
- GCB:
-
Germinal center B-cell
- GFR:
-
Growth factor receptors
- GLUT:
-
Glucose transporter protein type
- GO:
-
Gene Ontology
- GSEA:
-
Gene Set Enrichment Analysis
- H3K27:
-
Histone H3 lysine 27
- H3K4:
-
Histone H3 lysine 4
- Hb:
-
Hemoglobin
- HD-MTX:
-
High-dose methotrexate
- HP:
-
H. pylori
- HR:
-
Hazard ratio
- IELSG:
-
International Extranodal Lymphoma Study Group
- IL-10:
-
Interleukin-10
- IL1R:
-
Interleukin 1 receptor
- IMVD:
-
Intratumoral microvessel density
- IPI:
-
International Prognostic Index
- JAK/STAT:
-
Janus-associated kinase/signal transducer and activator of transcription
- KEGG:
-
Kyoto Encyclopedia of Genes and Genomes
- KPS:
-
Karnofsky performance score
- L3-SMI:
-
L3 lumbar-skeletal muscle index
- LDH:
-
Lactate dehydrogenase
- LLR:
-
Lactate dehydrogenase/lymphocyte ratio
- LMP1:
-
Latent membrane protein 1
- LMR:
-
Lymphocyte/monocyte ratio
- miRNA:
-
MicroRNA
- MALT:
-
Mucosa-associated lymphoid tissue
- MF:
-
Mycosis fungoides
- MHC:
-
Major histocompatibility complex
- MMSE:
-
Mini-Mental State Examination
- MSKCC:
-
Memorial Sloan-Kettering Cancer Center score
- MTOR:
-
Mammalian target of rapamycin
- MYD88:
-
Myeloid differentiation major response gene
- NF-κB:
-
Nuclear factor-kappaB
- NGS:
-
Next-generation sequencing
- NLR:
-
Neutrophil/lymphocyte ratio
- NKTCL-NT:
-
Natural killer/T-cell lymphoma (nasal type)
- OS:
-
Overall survival
- PCNSL:
-
Primary central nervous system lymphoma
- PD-1:
-
Programmed cell death-1
- PD-L1:
-
Programmed cell death-ligand1
- PD-L2:
-
Programmed death-ligand 2
- PFS:
-
Progression-free survival
- PI3K:
-
Phosphatidylinositol-3 kinase
- PTCL:
-
Peripheral T cell lymphoma
- RNU2-1f:
-
U2 small ribonucleic acid fragment
- SEER:
-
Surveillance, Epidemiology, and End Results
- SII:
-
Systemic immune inflammatory index
- snRNA:
-
Small nuclear RNA
- SUV:
-
Standardized uptake value
- TBIL:
-
Total bilirubin
- TCR:
-
T-cell receptors
- TLR:
-
Toll-like receptor
- TGF:
-
Transforming growth factor
- Th:
-
T-helper
- TMT:
-
Temporalis muscle thickness
- TNFR:
-
Tumor necrosis factor-α receptor
- WBRT:
-
Whole brain radiotherapy
References
Groves FD, Linet MS, Travis LB, Devesa SS. Cancer surveillance series: non-Hodgkin’s lymphoma incidence by histologic subtype in the United States from 1978 through 1995. J Natl Cancer Inst. 2000;92(15):1240–51. https://doi.org/10.1093/jnci/92.15.1240.
Paes FM, Kalkanis DG, Sideras PA, Serafini AN. FDG PET/CT of extranodal involvement in non-Hodgkin lymphoma and Hodgkin disease. Radiographics. 2010;30(1):269–91. https://doi.org/10.1148/rg.301095088.
Heckendorn E, Auerbach A. Pathology of extranodal lymphoma. Radiol Clin North Am. 2016;54(4):639–48. https://doi.org/10.1016/j.rcl.2016.03.001.
Castillo JJ, Winer ES, Olszewski AJ. Sites of extranodal involvement are prognostic in patients with diffuse large B-cell lymphoma in the rituximab era: an analysis of the Surveillance, Epidemiology and End Results database. Am J Hematol. 2014;89(3):310–4. https://doi.org/10.1002/ajh.23638.
Reginelli A, Urraro F, Sangiovanni A, Russo GM, Russo C, Grassi R, et al. Extranodal lymphomas: a pictorial review for CT and MRI classification. Acta Biomed. 2020;91(8-s):34–42. https://doi.org/10.23750/abm.v91i8-S.9971.
Ollila TA, Olszewski AJ. Extranodal diffuse large B cell lymphoma: molecular features, prognosis, and risk of central nervous system recurrence. Curr Treat Options Oncol. 2018;19(8):38. https://doi.org/10.1007/s11864-018-0555-8.
Taal BG, den Hartog Jager FCA, Burgers JMV, van Heerde P, Tio TL. Primary non-Hodgkin’s lymphoma of the stomach: Changing aspects and therapeutic choices. Eur J Cancer Clin Oncol. 1989;25(3):439–50. https://doi.org/10.1016/0277-5379(89)90256-3.
Arber DA, Orazi A, Hasserjian R, Thiele J, Borowitz MJ, Le Beau MM, et al. The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia. Blood. 2016;127(20):2391–405. https://doi.org/10.1182/blood-2016-03-643544.
Coiffier B. State-of-the-art therapeutics: diffuse large B-cell lymphoma. J Clin Oncol. 2005;23(26):6387–93. https://doi.org/10.1200/jco.2005.05.015.
Gonzalez VJ. Role of radiation therapy in the treatment of hodgkin lymphoma. Curr Hematol Malig Rep. 2017;12(3):244–50. https://doi.org/10.1007/s11899-017-0385-y.
Di Rocco A, Petrucci L, Assanto GM, Martelli M, Pulsoni A. Extranodal marginal zone lymphoma: pathogenesis, diagnosis and treatment. Cancers (Basel). 2022;14(7):1742. https://doi.org/10.3390/cancers14071742.
Zain J, Kallam A. Challenges in nodal peripheral T-cell lymphomas: from biological advances to clinical applicability. Front Oncol. 2023;13:1150715. https://doi.org/10.3389/fonc.2023.1150715.
Tian XP, Cao Y, Cai J, Zhang YC, Zou QH, Wang JN, et al. Novel target and treatment agents for natural killer/T-cell lymphoma. J Hematol Oncol. 2023;16(1):78. https://doi.org/10.1186/s13045-023-01483-9.
Hernández-Verdin I, Morales-Martínez A, Hoang-Xuan K, Alentorn A. Primary central nervous system lymphoma: advances in its pathogenesis, molecular markers and targeted therapies. Curr Opin Neurol. 2022;35(6):779–86. https://doi.org/10.1097/wco.0000000000001115.
Lebrun L, Allard-Demoustiez S, Salmon I. Pathology and new insights in central nervous system lymphomas. Curr Opin Oncol. 2023. https://doi.org/10.1097/cco.0000000000000978.
Yu L, Li L, Medeiros LJ, Young KH. NF-κB signaling pathway and its potential as a target for therapy in lymphoid neoplasms. Blood Rev. 2017;31(2):77–92. https://doi.org/10.1016/j.blre.2016.10.001.
Sun R-F, Yu Q-Q, Young KH. Critically dysregulated signaling pathways and clinical utility of the pathway biomarkers in lymphoid malignancies. Chronic Dis Transl Med. 2018;4(1):29–44. https://doi.org/10.1016/j.cdtm.2018.02.001.
Ramadass V, Vaiyapuri T, Tergaonkar V. Small molecule NF-κB pathway inhibitors in clinic. Int J Mol Sci. 2020;21(14):5164. https://doi.org/10.3390/ijms21145164.
Liu J, Liang L, Li D, Nong L, Zheng Y, Huang S, et al. JAK3/STAT3 oncogenic pathway and PRDM1 expression stratify clinicopathologic features of extranodal NK/T-cell lymphoma, nasal type. Oncol Rep. 2019;41(6):3219–32. https://doi.org/10.3892/or.2019.7112.
Kaulen LD, Denisova E, Hinz F, Hai L, Friedel D, Henegariu O, et al. Integrated genetic analyses of immunodeficiency-associated Epstein-Barr virus- (EBV) positive primary CNS lymphomas. Acta Neuropathol. 2023. https://doi.org/10.1007/s00401-023-02613-w.
Han Z, Wu X, Qin H, Yuan YC, Schmolze D, Su C, et al. Reprogramming of PD-1+ M2-like tumor-associated macrophages with anti-PD-L1 and lenalidomide in cutaneous T cell lymphoma. JCI Insight. 2023;8(13):e163518.https://doi.org/10.1172/jci.insight.163518.
Gao X, Kady N, Wang C, Abdelrahman S, Gann P, Sverdlov M, et al. Targeting lymphoma-associated macrophage expansion via CSF1R/JAK inhibition is a therapeutic vulnerability in peripheral T-cell lymphomas. Cancer Res Commun. 2022;2(12):1727–37. https://doi.org/10.1158/2767-9764.Crc-22-0336.
Xie W, Medeiros LJ, Li S, Tang G, Fan G, Xu J. PD-1/PD-L1 pathway: a therapeutic target in CD30+ large cell lymphomas. Biomedicines. 2022;10(7):1587. https://doi.org/10.3390/biomedicines10071587.
Gluud M, Pallesen EMH, Buus TB, Gjerdrum LMR, Lindahl LM, Kamstrup MR, et al. Malignant T cells induce skin barrier defects through cytokine-mediated JAK/STAT signaling in cutaneous T-cell lymphoma. Blood. 2023;141(2):180–93. https://doi.org/10.1182/blood.2022016690.
Beer-Hammer S, Zebedin E, von Holleben M, Alferink J, Reis B, Dresing P, et al. The catalytic PI3K isoforms p110gamma and p110delta contribute to B cell development and maintenance, transformation, and proliferation. J Leukoc Biol. 2010;87(6):1083–95. https://doi.org/10.1189/jlb.0809585.
Webb LM, Vigorito E, Wymann MP, Hirsch E, Turner M. Cutting edge: T cell development requires the combined activities of the p110gamma and p110delta catalytic isoforms of phosphatidylinositol 3-kinase. J Immunol. 2005;175(5):2783–7. https://doi.org/10.4049/jimmunol.175.5.2783.
Horwitz SM, Koch R, Porcu P, Oki Y, Moskowitz A, Perez M, et al. Activity of the PI3K-δ, γ inhibitor duvelisib in a phase 1 trial and preclinical models of T-cell lymphoma. Blood. 2018;131(8):888–98. https://doi.org/10.1182/blood-2017-08-802470.
Kim N, Saudemont A, Webb L, Camps M, Ruckle T, Hirsch E, et al. The p110delta catalytic isoform of PI3K is a key player in NK-cell development and cytokine secretion. Blood. 2007;110(9):3202–8. https://doi.org/10.1182/blood-2007-02-075366.
Saudemont A, Garçon F, Yadi H, Roche-Molina M, Kim N, Segonds-Pichon A, et al. P110gamma and p110delta isoforms of phosphoinositide 3-kinase differentially regulate natural killer cell migration in health and disease. Proc Natl Acad Sci U S A. 2009;106(14):5795–800. https://doi.org/10.1073/pnas.0808594106.
Gopal AK, Kahl BS, de Vos S, Wagner-Johnston ND, Schuster SJ, Jurczak WJ, et al. PI3Kδ inhibition by idelalisib in patients with relapsed indolent lymphoma. N Engl J Med. 2014;370(11):1008–18. https://doi.org/10.1056/NEJMoa1314583.
Vangapandu HV, Jain N, Gandhi V. Duvelisib: a phosphoinositide-3 kinase δ/γ inhibitor for chronic lymphocytic leukemia. Expert Opin Investig Drugs. 2017;26(5):625–32. https://doi.org/10.1080/13543784.2017.1312338.
Dreyling M, Santoro A, Mollica L, Leppä S, Follows GA, Lenz G, et al. Phosphatidylinositol 3-kinase inhibition by copanlisib in relapsed or Rrefractory indolent lymphoma. J Clin Oncol. 2017;35(35):3898–905. https://doi.org/10.1200/jco.2017.75.4648.
Grommes C, Pentsova E, Schaff LR, Nolan CP, Kaley T, Reiner AS et al. Preclinical and clinical evaluation of Buparlisib (BKM120) in recurrent/refractory Central Nervous System Lymphoma. Leuk Lymphoma. 2023:1–9. https://doi.org/10.1080/10428194.2023.2223734.
Huang D, Song TL, Nairismägi ML, Laurensia Y, Pang WL, Zhe DCM, et al. Evaluation of the PIK3 pathway in peripheral T-cell lymphoma and NK/T-cell lymphoma. Br J Haematol. 2020;189(4):731–44. https://doi.org/10.1111/bjh.16435.
Oka T, Miyagaki T. Novel and future therapeutic drugs for advanced mycosis fungoides and sézary syndrome. Front Med (Lausanne). 2019;6:116. https://doi.org/10.3389/fmed.2019.00116.
Zhang GH, Miao FA, Xu JG, Zhang Y. Angiotensin II enhances the proliferation of Natural Killer/T-cell lymphoma cells via activating PI3K/Akt signaling pathway. Biosci Rep. 2020;40(10):1. https://doi.org/10.1042/BSR20202388.
Petrich AM, Leshchenko V, Kuo PY, Xia B, Thirukonda VK, Ulahannan N, et al. Akt inhibitors MK-2206 and nelfinavir overcome mTOR inhibitor resistance in diffuse large B-cell lymphoma. Clin Cancer Res. 2012;18(9):2534–44. https://doi.org/10.1158/1078-0432.Ccr-11-1407.
Renaud L, Bossard JB, Carpentier B, Terriou L, Cambier N, Chanteau G, et al. Treatment with temozolomide and ibrutinib in recurrent/refractory primary (PCNSL) and secondary CNS lymphoma (SCNSL). Eur J Haematol. 2021;107(3):370–3. https://doi.org/10.1111/ejh.13667.
Westin JR. Status of PI3K/Akt/mTOR pathway inhibitors in lymphoma. Clin Lymphoma Myeloma Leuk. 2014;14(5):335–42. https://doi.org/10.1016/j.clml.2014.01.007.
Korfel A, Schlegel U, Herrlinger U, Dreyling M, Schmidt C, von Baumgarten L, et al. Phase II Trial of temsirolimus for relapsed/refractory primary CNS lymphoma. J Clin Oncol. 2016;34(15):1757–63. https://doi.org/10.1200/jco.2015.64.9897.
Yokogami K, Azuma M, Takeshima H, Hirai T. Lymphomas of central nervous system. Adv Exp Med Biol. 2023;1405:527–43. https://doi.org/10.1007/978-3-031-23705-8_20.
Bresin A, Cristofoletti C, Caprini E, Cantonetti M, Monopoli A, Russo G, et al. Preclinical evidence for targeting PI3K/mTOR signaling with dual-inhibitors as a therapeutic strategy against cutaneous T-cell lymphoma. J Invest Dermatol. 2020;140(5):1045-53.e6. https://doi.org/10.1016/j.jid.2019.08.454.
Kim SJ, Shin DY, Kim JS, Yoon DH, Lee WS, Lee H, et al. A phase II study of everolimus (RAD001), an mTOR inhibitor plus CHOP for newly diagnosed peripheral T-cell lymphomas. Ann Oncol. 2016;27(4):712–8. https://doi.org/10.1093/annonc/mdv624.
Kawada J, Ito Y, Iwata S, Suzuki M, Kawano Y, Kanazawa T, et al. mTOR inhibitors induce cell-cycle arrest and inhibit tumor growth in Epstein-Barr virus-associated T and natural killer cell lymphoma cells. Clin Cancer Res. 2014;20(21):5412–22. https://doi.org/10.1158/1078-0432.Ccr-13-3172.
Ng SB, Selvarajan V, Huang G, Zhou J, Feldman AL, Law M, et al. Activated oncogenic pathways and therapeutic targets in extranodal nasal-type NK/T cell lymphoma revealed by gene expression profiling. J Pathol. 2011;223(4):496–510. https://doi.org/10.1002/path.2823.
Ng SB, Yan J, Huang G, Selvarajan V, Tay JL, Lin B, et al. Dysregulated microRNAs affect pathways and targets of biologic relevance in nasal-type natural killer/T-cell lymphoma. Blood. 2011;118(18):4919–29. https://doi.org/10.1182/blood-2011-07-364224.
Gomes Candido Reis D, Levy D, Lage LAdPC, Culler HF, Rocha V, Bydlowski SP, et al. New genetic prognostic biomarkers in primary central nervous system lymphoma (PCNSL). Brain Behav. 2021;11(4):e02061. https://doi.org/10.1002/brb3.2061.
Farmah P, Mehta AH, Vu AH, Tchokouani LS, Nazir S. Extranodal marginal zone mucosa-associated lymphoid tissue lymphoma of the gallbladder: a case report and literature review. Cureus. 2023;15(3):e35825. https://doi.org/10.7759/cureus.35825.
Xu S, Ren J, Lewis JM, Carlson KR, Girardi M. Proteasome inhibitors interact synergistically with BCL2, histone deacetylase, BET, and Jak inhibitors against cutaneous T-cell lymphoma cells. J Invest Dermatol. 2023;143(7):1322-5.e3. https://doi.org/10.1016/j.jid.2022.12.017.
Cayrol F, Praditsuktavorn P, Fernando TM, Kwiatkowski N, Marullo R, Calvo-Vidal MN, et al. THZ1 targeting CDK7 suppresses STAT transcriptional activity and sensitizes T-cell lymphomas to BCL2 inhibitors. Nat Commun. 2017;8:14290. https://doi.org/10.1038/ncomms14290.
Ng SB, Fan S, Choo SN, Hoppe M, Mai Phuong H, De Mel S, et al. Quantitative analysis of a multiplexed immunofluorescence panel in T-cell lymphoma. SLAS Technol. 2018;23(3):252–8. https://doi.org/10.1177/2472630317747197.
Ying L, Liu P, Ding Z, Wray-McCann G, Emery J, Colon N, et al. Anti-CD40L therapy prevents the formation of precursor lesions to gastric B-cell MALT lymphoma in a mouse model. J Pathol. 2023;259(4):402–14. https://doi.org/10.1002/path.6053.
Tao R, Fan L, Song Y, Hu Y, Zhang W, Wang Y, et al. Sintilimab for relapsed/refractory extranodal NK/T cell lymphoma: a multicenter, single-arm, phase 2 trial (ORIENT-4). Signal Transduct Target Ther. 2021;6(1):365. https://doi.org/10.1038/s41392-021-00768-0.
Lesokhin AM, Ansell SM, Armand P, Scott EC, Halwani A, Gutierrez M, et al. Nivolumab in patients with relapsed or refractory hematologic malignancy: preliminary results of a phase Ib study. J Clin Oncol. 2016;34(23):2698–704. https://doi.org/10.1200/jco.2015.65.9789.
Kwong YL, Chan TSY, Tan D, Kim SJ, Poon LM, Mow B, et al. PD1 blockade with pembrolizumab is highly effective in relapsed or refractory NK/T-cell lymphoma failing l-asparaginase. Blood. 2017;129(17):2437–42. https://doi.org/10.1182/blood-2016-12-756841.
Nayak L, Iwamoto FM, LaCasce A, Mukundan S, Roemer MGM, Chapuy B, et al. PD-1 blockade with nivolumab in relapsed/refractory primary central nervous system and testicular lymphoma. Blood. 2017;129(23):3071–3. https://doi.org/10.1182/blood-2017-01-764209.
Nakamura T, Tateishi K, Niwa T, Matsushita Y, Tamura K, Kinoshita M, et al. Recurrent mutations of CD79B and MYD88 are the hallmark of primary central nervous system lymphomas. Neuropathol Appl Neurobiol. 2016;42(3):279–90. https://doi.org/10.1111/nan.12259.
Zhou Y, Liu W, Xu Z, Zhu H, Xiao D, Su W, et al. Analysis of genomic alteration in primary central nervous system lymphoma and the expression of some related genes. Neoplasia (New York, NY). 2018;20(10):1059–69. https://doi.org/10.1016/j.neo.2018.08.012.
Shaffer AL 3rd, Young RM, Staudt LM. Pathogenesis of human B cell lymphomas. Annu Rev Immunol. 2012;30:565–610. https://doi.org/10.1146/annurev-immunol-020711-075027.
Davis RE, Ngo VN, Lenz G, Tolar P, Young RM, Romesser PB, et al. Chronic active B-cell-receptor signalling in diffuse large B-cell lymphoma. Nature. 2010;463(7277):88–92. https://doi.org/10.1038/nature08638.
Carty SA, Murga-Zamalloa CA, Wilcox RA. SOHO state of the art updates and next questions | new pathways and new targets in PTCL: staying on target. Clin Lymphoma Myeloma Leuk. 2023;23(8):561–74. https://doi.org/10.1016/j.clml.2023.04.007.
Umakanthan JM, Iqbal J, Batlevi CL, Bouska A, Smith LM, Shostrom V, et al. Phase I/II study of dasatinib and exploratory genomic analysis in relapsed or refractory non-Hodgkin lymphoma. Br J Haematol. 2019;184(5):744–52. https://doi.org/10.1111/bjh.15702.
Carty SA, Murga-Zamalloa CA, Wilcox RA. SOHO state of the art updates and next questions new pathways and new targets in PTCL: staying on target. Clin Lymphoma Myeloma Leuk. 2023;23(8):561–74. https://doi.org/10.1016/j.clml.2023.04.007.
Nakamura S, Matsumoto T, Iida M, Yao T, Tsuneyoshi M. Primary gastrointestinal lymphoma in Japan: a clinicopathologic analysis of 455 patients with special reference to its time trends. Cancer. 2003;97(10):2462–73. https://doi.org/10.1002/cncr.11415.
Nakamura S, Matsumoto T, Ye H, Nakamura S, Suekane H, Matsumoto H, et al. Helicobacter pylori-negative gastric mucosa-associated lymphoid tissue lymphoma: a clinicopathologic and molecular study with reference to antibiotic treatment. Cancer. 2006;107(12):2770–8. https://doi.org/10.1002/cncr.22326.
Hauer AC, Finn TM, MacDonald TT, Spencer J, Isaacson PG. Analysis of TH1 and TH2 cytokine production in low grade B cell gastric MALT-type lymphomas stimulated in vitro with Helicobacter pylori. J Clin Pathol. 1997;50(11):957–9. https://doi.org/10.1136/jcp.50.11.957.
Deutsch AJ, Steinbauer E, Hofmann NA, Strunk D, Gerlza T, Beham-Schmid C, et al. Chemokine receptors in gastric MALT lymphoma: loss of CXCR4 and upregulation of CXCR7 is associated with progression to diffuse large B-cell lymphoma. Mod Pathol. 2013;26(2):182–94. https://doi.org/10.1038/modpathol.2012.134.
Mazzucchelli L, Blaser A, Kappeler A, Schärli P, Laissue JA, Baggiolini M, et al. BCA-1 is highly expressed in helicobacter pylori-induced mucosa-associated lymphoid tissue and gastric lymphoma. J Clin Invest. 1999;104(10):R49-54. https://doi.org/10.1172/jci7830.
Kuo SH, Wu MS, Yeh KH, Lin CW, Hsu PN, Chen LT. Novel insights of lymphomagenesis of Helicobacter pylori-dependent gastric mucosa-associated lymphoid tissue lymphoma. Cancers (Basel). 2019;11(4):547. https://doi.org/10.3390/cancers11040547.
Noy A, de Vos S, Thieblemont C, Martin P, Flowers CR, Morschhauser F, et al. Targeting bruton tyrosine kinase with ibrutinib in relapsed/refractory marginal zone lymphoma. Blood. 2017;129(16):2224–32. https://doi.org/10.1182/blood-2016-10-747345.
Dreyling M, Santoro A, Mollica L, Leppä S, Follows GA, Lenz G, et al. Phosphatidylinositol 3-kinase inhibition by copanlisib in relapsed or refractory indolent lymphoma. J Clin Oncol. 2017;35(35):3898–905. https://doi.org/10.1200/jco.2017.75.4648.
Nakamura S, Matsumoto T, Nakamura S, Jo Y, Fujisawa K, Suekane H, et al. Chromosomal translocation t(11;18)(q21;q21) in gastrointestinal mucosa associated lymphoid tissue lymphoma. J Clin Pathol. 2003;56(1):36–42. https://doi.org/10.1136/jcp.56.1.36.
Sagaert X, Tousseyn T, Vanhentenrijk V, Van Loo P, Baens M, Marynen P, et al. Comparative expressed sequence hybridization studies of t(11;18)(q21;q21)-positive and -negative gastric MALT lymphomas reveal both unique and overlapping gene programs. Mod Pathol. 2010;23(3):458–69. https://doi.org/10.1038/modpathol.2009.182.
Taal BG, Burgers JM. Primary non-Hodgkin’s lymphoma of the stomach: endoscopic diagnosis and the role of surgery. Scand J Gastroenterol Suppl. 1991;188:33–7. https://doi.org/10.3109/00365529109111227.
Dmitrieva A, Kozlova O, Atuchin V, Milentieva I, Vesnina A, Ivanova S, et al. Study of the effect of baicalin from scutellaria baicalensis on the gastrointestinal tract normoflora and helicobacter pylori. Int J Mol Sci. 2023;24(15):11906. https://doi.org/10.3390/ijms241511906.
Lemaitre M, Brice P, Frigeni M, Hermine O, Arcaini L, Thieblemont C, et al. Hepatitis B virus-associated b-cell non-hodgkin lymphoma in non-endemic areas in western europe: clinical characteristics and prognosis. J Infect. 2020;80(2):219–24. https://doi.org/10.1016/j.jinf.2019.12.005.
Armand M, Besson C, Hermine O, Davi F. Hepatitis C virus - associated marginal zone lymphoma. Best Pract Res Clin Haematol. 2017;30(1–2):41–9. https://doi.org/10.1016/j.beha.2017.02.001.
Liu H, Ye H, Ruskone-Fourmestraux A, De Jong D, Pileri S, Thiede C, et al. T(11;18) is a marker for all stage gastric MALT lymphomas that will not respond to H. pylori eradication. Gastroenterology. 2002;122(5):1286–94. https://doi.org/10.1053/gast.2002.33047.
Nakamura S, Sugiyama T, Matsumoto T, Iijima K, Ono S, Tajika M, et al. Long-term clinical outcome of gastric MALT lymphoma after eradication of Helicobacter pylori: a multicentre cohort follow-up study of 420 patients in Japan. Gut. 2012;61(4):507–13. https://doi.org/10.1136/gutjnl-2011-300495.
Wirth A, Gospodarowicz M, Aleman BM, Bressel M, Ng A, Chao M, et al. Long-term outcome for gastric marginal zone lymphoma treated with radiotherapy: a retrospective, multi-centre, International Extranodal Lymphoma Study Group study. Ann Oncol. 2013;24(5):1344–51. https://doi.org/10.1093/annonc/mds623.
Zucca E, Conconi A, Martinelli G, Bouabdallah R, Tucci A, Vitolo U, et al. Final results of the IELSG-19 randomized trial of mucosa-associated lymphoid tissue lymphoma: improved event-free and progression-free survival with rituximab plus chlorambucil versus either chlorambucil or rituximab monotherapy. J Clin Oncol. 2017;35(17):1905–12. https://doi.org/10.1200/jco.2016.70.6994.
Willemze R, Cerroni L, Kempf W, Berti E, Facchetti F, Swerdlow SH, et al. The 2018 update of the WHO-EORTC classification for primary cutaneous lymphomas. Blood. 2019;133(16):1703–14. https://doi.org/10.1182/blood-2018-11-881268.
Lee HJ, Im JG, Goo JM, Kim KW, Choi BI, Chang KH, et al. Peripheral T-cell lymphoma: spectrum of imaging findings with clinical and pathologic features. Radiographics. 2003;23(1):7–26. https://doi.org/10.1148/rg.231025018. discussion -8.
Jones CL, Degasperi A, Grandi V, Amarante TD, Mitchell TJ, Nik-Zainal S, et al. Spectrum of mutational signatures in T-cell lymphoma reveals a key role for UV radiation in cutaneous T-cell lymphoma. Sci Rep. 2021;11(1):3962. https://doi.org/10.1038/s41598-021-83352-4.
Bakr FS, Whittaker SJ. Advances in the understanding and treatment of Cutaneous T-cell Lymphoma. Front Oncol. 2022;12:1043254. https://doi.org/10.3389/fonc.2022.1043254.
Zinzani PL, Musuraca G, Tani M, Stefoni V, Marchi E, Fina M, et al. Phase II trial of proteasome inhibitor bortezomib in patients with relapsed or refractory cutaneous T-cell lymphoma. J Clin Oncol. 2007;25(27):4293–7. https://doi.org/10.1200/jco.2007.11.4207.
Kiel MJ, Sahasrabuddhe AA, Rolland DCM, Velusamy T, Chung F, Schaller M, et al. Genomic analyses reveal recurrent mutations in epigenetic modifiers and the JAK-STAT pathway in Sézary syndrome. Nat Commun. 2015;6:8470. https://doi.org/10.1038/ncomms9470.
Iyer A, Hennessey D, O’Keefe S, Patterson J, Wang W, Wong GK, et al. Branched evolution and genomic intratumor heterogeneity in the pathogenesis of cutaneous T-cell lymphoma. Blood Adv. 2020;4(11):2489–500. https://doi.org/10.1182/bloodadvances.2020001441.
Bradford PT, Devesa SS, Anderson WF, Toro JR. Cutaneous lymphoma incidence patterns in the United States: a population-based study of 3884 cases. Blood. 2009;113(21):5064–73. https://doi.org/10.1182/blood-2008-10-184168.
Kim EJ, Hess S, Richardson SK, Newton S, Showe LC, Benoit BM, et al. Immunopathogenesis and therapy of cutaneous T cell lymphoma. J Clin Invest. 2005;115(4):798–812. https://doi.org/10.1172/jci24826.
Quaglino P, Maule M, Prince HM, Porcu P, Horwitz S, Duvic M, et al. Global patterns of care in advanced stage mycosis fungoides/Sezary syndrome: a multicenter retrospective follow-up study from the Cutaneous Lymphoma International Consortium. Ann Oncol. 2017;28(10):2517–25. https://doi.org/10.1093/annonc/mdx352.
Hughes CFM, Khot A, McCormack C, Lade S, Westerman DA, Twigger R, et al. Lack of durable disease control with chemotherapy for mycosis fungoides and Sézary syndrome: a comparative study of systemic therapy. Blood. 2015;125(1):71–81. https://doi.org/10.1182/blood-2014-07-588236.
Jiang L, Gu ZH, Yan ZX, Zhao X, Xie YY, Zhang ZG, et al. Exome sequencing identifies somatic mutations of DDX3X in natural killer/T-cell lymphoma. Nat Genet. 2015;47(9):1061–6. https://doi.org/10.1038/ng.3358.
Bassig BA, Au WY, Mang O, Ngan R, Morton LM, Ip DK, et al. Subtype-specific incidence rates of lymphoid malignancies in Hong Kong compared to the United States, 2001–2010. Cancer Epidemiol. 2016;42:15–23. https://doi.org/10.1016/j.canep.2016.02.007.
Tse E, Kwong YL. The diagnosis and management of NK/T-cell lymphomas. J Hematol Oncol. 2017;10(1):85. https://doi.org/10.1186/s13045-017-0452-9.
Lin GW, Xu C, Chen K, Huang HQ, Chen J, Song B, et al. Genetic risk of extranodal natural killer T-cell lymphoma: a genome-wide association study in multiple populations. Lancet Oncol. 2020;21(2):306–16. https://doi.org/10.1016/s1470-2045(19)30799-5.
Kimura H. EBV in T-/NK-Cell tumorigenesis. Adv Exp Med Biol. 2018;1045:459–75. https://doi.org/10.1007/978-981-10-7230-7_21.
Oishi N, Satou A, Miyaoka M, Kawashima I, Segawa T, Miyake K, et al. Genetic and immunohistochemical profiling of NK/T-cell lymphomas reveals prognostically relevant BCOR-MYC association. Blood Adv. 2023;7(1):178–89. https://doi.org/10.1182/bloodadvances.2022007541.
Song TL, Nairismägi ML, Laurensia Y, Lim JQ, Tan J, Li ZM, et al. Oncogenic activation of the STAT3 pathway drives PD-L1 expression in natural killer/T-cell lymphoma. Blood. 2018;132(11):1146–58. https://doi.org/10.1182/blood-2018-01-829424.
de Mel S, Hue SS, Jeyasekharan AD, Chng WJ, Ng SB. Molecular pathogenic pathways in extranodal NK/T cell lymphoma. J Hematol Oncol. 2019;12(1):33. https://doi.org/10.1186/s13045-019-0716-7.
Yang Y, Cao JZ, Lan SM, Wu JX, Wu T, Zhu SY, et al. Association of improved locoregional control with prolonged survival in early-stage extranodal nasal-type natural killer/T-cell lymphoma. JAMA Oncol. 2017;3(1):83–91. https://doi.org/10.1001/jamaoncol.2016.5094.
Deng XW, Wu JX, Wu T, Zhu SY, Shi M, Su H, et al. Radiotherapy is essential after complete response to asparaginase-containing chemotherapy in early-stage extranodal nasal-type NK/T-cell lymphoma: A multicenter study from the China Lymphoma Collaborative Group (CLCG). Radiother Oncol. 2018;129(1):3–9. https://doi.org/10.1016/j.radonc.2018.04.026.
Yang Y, Zhu Y, Cao JZ, Zhang YJ, Xu LM, Yuan ZY, et al. Risk-adapted therapy for early-stage extranodal nasal-type NK/T-cell lymphoma: analysis from a multicenter study. Blood. 2015;126(12):1424–32. https://doi.org/10.1182/blood-2015-04-639336. quiz 517.
Yong W, Zheng W, Zhu J, Zhang Y, Wang X, Xie Y, et al. L-asparaginase in the treatment of refractory and relapsed extranodal NK/T-cell lymphoma, nasal type. Ann Hematol. 2009;88(7):647–52. https://doi.org/10.1007/s00277-008-0669-3.
Li X, Cheng Y, Zhang M, Yan J, Li L, Fu X, et al. Activity of pembrolizumab in relapsed/refractory NK/T-cell lymphoma. J Hematol Oncol. 2018;11(1):15. https://doi.org/10.1186/s13045-018-0559-7.
Jaccard A, Gachard N, Marin B, Rogez S, Audrain M, Suarez F, et al. Efficacy of L-asparaginase with methotrexate and dexamethasone (AspaMetDex regimen) in patients with refractory or relapsing extranodal NK/T-cell lymphoma, a phase 2 study. Blood. 2011;117(6):1834–9. https://doi.org/10.1182/blood-2010-09-307454.
Lee J, Au WY, Park MJ, Suzumiya J, Nakamura S, Kameoka J, et al. Autologous hematopoietic stem cell transplantation in extranodal natural killer/T cell lymphoma: a multinational, multicenter, matched controlled study. Biol Blood Marrow Transplant. 2008;14(12):1356–64. https://doi.org/10.1016/j.bbmt.2008.09.014.
Wang J, Wei L, Ye J, Yang L, Li X, Cong J, et al. Autologous hematopoietic stem cell transplantation may improve long-term outcomes in patients with newly diagnosed extranodal natural killer/T-cell lymphoma, nasal type: a retrospective controlled study in a single center. Int J Hematol. 2018;107(1):98–104. https://doi.org/10.1007/s12185-017-2324-z.
Philippe Walter L, Couronné L, Jais JP, Nguyen PD, Blaise D, Pigneux A, et al. Outcome after hematopoietic stem cell transplantation in patients with extranodal natural killer/T-Cell lymphoma, nasal type: A French study from the Société Francophone de Greffe de Moelle et de Thérapie Cellulaire (SFGM-TC). Am J Hematol. 2021;96(7):834–45. https://doi.org/10.1002/ajh.26200.
Louis DN, Perry A, Wesseling P, Brat DJ, Cree IA, Figarella-Branger D, et al. The 2021 WHO classification of tumors of the central nervous system: a summary. Neuro Oncol. 2021;23(8):1231–51. https://doi.org/10.1093/neuonc/noab106.
Alaggio R, Amador C, Anagnostopoulos I, Attygalle AD, Araujo IBO, Berti E, et al. The the World Health Organization classification of haematolymphoid tumours: lymphoid neoplasms. Leukemia. 2022;36(7):1720–48. https://doi.org/10.1038/s41375-022-01620-2.
Bravetti C, Degaud M, Armand M, Sourdeau E, Mokhtari K, Maloum K, et al. Combining MYD88 L265P mutation detection and clonality determination on CSF cellular and cell-free DNA improves diagnosis of primary CNS lymphoma. Br J Haematol. 2023. https://doi.org/10.1111/bjh.18758.
Löw S, Han CH, Batchelor TT. Primary central nervous system lymphoma. Ther Adv Neurol Disord. 2018;11:1756286418793562. https://doi.org/10.1177/1756286418793562.
Schaff LR, Grommes C. Primary central nervous system lymphoma. Blood. 2022;140(9):971–9. https://doi.org/10.1182/blood.2020008377.
Farrall AL, Smith JR. Changing incidence and survival of primary central nervous system lymphoma in Australia: a 33-year national population-based study. Cancers (Basel). 2021;13(3):403. https://doi.org/10.3390/cancers13030403.
Puhakka I, Kuitunen H, Jäkälä P, Sonkajärvi E, Turpeenniemi-Hujanen T, Rönkä A, et al. Primary central nervous system lymphoma high incidence and poor survival in Finnish population-based analysis. BMC Cancer. 2022;22(1):236. https://doi.org/10.1186/s12885-022-09315-8.
Ghozy S, Dibas M, Afifi AM, Hashim MA, Abbas AS, Abdel-Daim MM, et al. Primary cerebral lymphoma’ characteristics, incidence, survival, and causes of death in the United States. J Neurol Sci. 2020;415:116890. https://doi.org/10.1016/j.jns.2020.116890.
Masouris I, Manz K, Pfirrmann M, Dreyling M, Angele B, Straube A, et al. CXCL13 and CXCL9 CSF levels in central nervous system lymphoma-diagnostic, therapeutic, and prognostic relevance. Front Neurol. 2021;12:654543. https://doi.org/10.3389/fneur.2021.654543.
Chukwueke U, Grommes C, Nayak L. Primary central nervous system lymphomas. Hematol Oncol Clin North Am. 2022;36(1):147–59. https://doi.org/10.1016/j.hoc.2021.09.004.
Camilleri-Broët S, Martin A, Moreau A, Angonin R, Hénin D, Gontier MF, et al. Primary central nervous system lymphomas in 72 immunocompetent patients: pathologic findings and clinical correlations. Groupe Ouest Est d’étude des Leucénies et Autres Maladies du Sang (GOELAMS). Am J Clin Pathol. 1998;110(5):607–12. https://doi.org/10.1093/ajcp/110.5.607.
Camilleri-Broët S, Crinière E, Broët P, Delwail V, Mokhtari K, Moreau A, et al. A uniform activated B-cell-like immunophenotype might explain the poor prognosis of primary central nervous system lymphomas: analysis of 83 cases. Blood. 2006;107(1):190–6. https://doi.org/10.1182/blood-2005-03-1024.
Hernández-Verdin I, Kirasic E, Wienand K, Mokhtari K, Eimer S, Loiseau H, et al. Molecular and clinical diversity in primary central nervous system lymphoma. Ann Oncol. 2023;34(2):186–99. https://doi.org/10.1016/j.annonc.2022.11.002.
Wright GW, Huang DW, Phelan JD, Coulibaly ZA, Roulland S, Young RM, et al. A probabilistic classification tool for genetic subtypes of diffuse large B cell lymphoma with therapeutic implications. Cancer Cell. 2020;37(4):551-68 e14. https://doi.org/10.1016/j.ccell.2020.03.015.
Alcantara M, Fuentealba J, Soussain C. Emerging landscape of immunotherapy for primary central nervous system lymphoma. Cancers (Basel). 2021;13(20):5061. https://doi.org/10.3390/cancers13205061.
Tateishi K, Miyake Y, Kawazu M, Sasaki N, Nakamura T, Sasame J, et al. A hyperactive RelA/p65-hexokinase 2 signaling axis drives primary central nervous system lymphoma. Cancer Res. 2020;80(23):5330–43. https://doi.org/10.1158/0008-5472.Can-20-2425.
Schmitz R, Wright GW, Huang DW, Johnson CA, Phelan JD, Wang JQ, et al. Genetics and pathogenesis of diffuse large B-cell lymphoma. N Engl J Med. 2018;378(15):1396–407. https://doi.org/10.1056/NEJMoa1801445.
Tateishi K, Miyake Y, Nakamura T, Yamamoto T. Primary central nervous system lymphoma: clinicopathological and genomic insights for therapeutic development. Brain Tumor Pathol. 2021;38(3):173–82. https://doi.org/10.1007/s10014-021-00408-z.
Nagane M. Molecular pathogenesis and therapeutic development of primary central nervous system lymphoma: update and future perspectives. Rinsho Ketsueki. 2022;63(9):1145–56. https://doi.org/10.11406/rinketsu.63.1145.
Jin Q, Jiang H, Han Y, Li C, Zhang L, Zhang Y, et al. Frequent gene mutations and their possible roles in the pathogenesis, treatment and prognosis of primary central nervous system lymphoma. World Neurosurg. 2023;170:99–106. https://doi.org/10.1016/j.wneu.2022.11.056.
Radke J, Ishaque N, Koll R, Gu Z, Schumann E, Sieverling L, et al. The genomic and transcriptional landscape of primary central nervous system lymphoma. Nat Commun. 2022;13(1):2558. https://doi.org/10.1038/s41467-022-30050-y.
Yamaguchi J, Ohka F, Lushun C, Motomura K, Aoki K, Takeuchi K, et al. CD79B Y196 mutation is a potent predictive marker for favorable response to R-MPV in primary central nervous system lymphoma. Cancer Med. 2023;12(6):7116–26. https://doi.org/10.1002/cam4.5512.
Zhu Q, Wang J, Zhang W, Zhu W, Wu Z, Chen Y, et al. Whole-genome/exome sequencing uncovers mutations and copy number variations in primary diffuse large B-cell lymphoma of the central nervous system. Front Genet. 2022;13:878618. https://doi.org/10.3389/fgene.2022.878618.
Alame M, Cornillot E, Cacheux V, Rigau V, Costes-Martineau V, Lacheretz-Szablewski V, et al. The immune contexture of primary central nervous system diffuse large B cell lymphoma associates with patient survival and specific cell signaling. Theranostics. 2021;11(8):3565–79. https://doi.org/10.7150/thno.54343.
Marcelis L, Antoranz A, Delsupehe AM, Biesemans P, Ferreiro JF, Debackere K, et al. In-depth characterization of the tumor microenvironment in central nervous system lymphoma reveals implications for immune-checkpoint therapy. Cancer Immunol Immunother. 2020;69(9):1751–66. https://doi.org/10.1007/s00262-020-02575-y.
Braggio E, Van Wier S, Ojha J, McPhail E, Asmann YW, Egan J, et al. Genome-wide analysis uncovers novel recurrent alterations in primary central nervous system lymphomas. Clin Cancer Res. 2015;21(17):3986–94. https://doi.org/10.1158/1078-0432.Ccr-14-2116.
Montesinos-Rongen M, Godlewska E, Brunn A, Wiestler OD, Siebert R, Deckert M. Activating L265P mutations of the MYD88 gene are common in primary central nervous system lymphoma. Acta Neuropathol. 2011;122(6):791–2. https://doi.org/10.1007/s00401-011-0891-2.
Montesinos-Rongen M, Schäfer E, Siebert R, Deckert M. Genes regulating the B cell receptor pathway are recurrently mutated in primary central nervous system lymphoma. Acta Neuropathol. 2012;124(6):905–6. https://doi.org/10.1007/s00401-012-1064-7.
Grommes C, Nayak L, Tun HW, Batchelor TT. Introduction of novel agents in the treatment of primary CNS lymphoma. Neuro Oncol. 2019;21(3):306–13. https://doi.org/10.1093/neuonc/noy193.
Grommes C, Pastore A, Palaskas N, Tang SS, Campos C, Schartz D, et al. Ibrutinib unmasks critical role of bruton tyrosine kinase in primary CNS lymphoma. Cancer Discov. 2017;7(9):1018–29. https://doi.org/10.1158/2159-8290.Cd-17-0613.
Sasaki N, Nagane M. Perspectives on precision medicine in primary central nervous system lymphoma. No Shinkei Geka. 2022;50(1):51–60. https://doi.org/10.11477/mf.1436204531.
Shen J, Liu J. Bruton’s tyrosine kinase inhibitors in the treatment of primary central nervous system lymphoma: A mini-review. Front Oncol. 2022;12:1034668. https://doi.org/10.3389/fonc.2022.1034668.
Steffanoni S, Batchelor TT. Targeting Bruton’s tyrosine kinase in primary central nervous system lymphoma. Curr Opin Neurol. 2021;34(6):848–56. https://doi.org/10.1097/wco.0000000000000993.
Wirsching HG, Weller M, Balabanov S, Roth P. Targeted therapies and immune checkpoint inhibitors in primary CNS lymphoma. Cancers (Basel). 2021;13(12):3073. https://doi.org/10.3390/cancers13123073.
Ge L, Xu L, Lu S, Yan H. Expression and function of toll-like receptor 10 (TLR10) in diffuse large B cell lymphoma, acute myeloid leukemia, and glioma. Med Sci Monit. 2020;26:e921500. https://doi.org/10.12659/msm.921500.
Hottinger AF, Alentorn A, Hoang-Xuan K. Recent developments and controversies in primary central nervous system lymphoma. Curr Opin Oncol. 2015;27(6):496–501. https://doi.org/10.1097/cco.0000000000000233.
Chapuy B, Roemer MG, Stewart C, Tan Y, Abo RP, Zhang L, et al. Targetable genetic features of primary testicular and primary central nervous system lymphomas. Blood. 2016;127(7):869–81. https://doi.org/10.1182/blood-2015-10-673236.
Montesinos-Rongen M, Zühlke-Jenisch R, Gesk S, Martín-Subero JI, Schaller C, Van Roost D, et al. Interphase cytogenetic analysis of lymphoma-associated chromosomal breakpoints in primary diffuse large B-cell lymphomas of the central nervous system. J Neuropathol Exp Neurol. 2002;61(10):926–33. https://doi.org/10.1093/jnen/61.10.926.
Montesinos-Rongen M, Akasaka T, Zühlke-Jenisch R, Schaller C, Van Roost D, Wiestler OD, et al. Molecular characterization of BCL6 breakpoints in primary diffuse large B-cell lymphomas of the central nervous system identifies GAPD as novel translocation partner. Brain Pathol. 2003;13(4):534–8. https://doi.org/10.1111/j.1750-3639.2003.tb00483.x.
Shen DF, Zhuang Z, LeHoang P, Böni R, Zheng S, Nussenblatt RB, et al. Utility of microdissection and polymerase chain reaction for the detection of immunoglobulin gene rearrangement and translocation in primary intraocular lymphoma. Ophthalmology. 1998;105(9):1664–9. https://doi.org/10.1016/s0161-6420(98)99036-4.
Montesinos-Rongen M, Van Roost D, Schaller C, Wiestler OD, Deckert M. Primary diffuse large B-cell lymphomas of the central nervous system are targeted by aberrant somatic hypermutation. Blood. 2004;103(5):1869–75. https://doi.org/10.1182/blood-2003-05-1465.
Montesinos-Rongen M, Schmitz R, Courts C, Stenzel W, Bechtel D, Niedobitek G, et al. Absence of immunoglobulin class switch in primary lymphomas of the central nervous system. Am J Pathol. 2005;166(6):1773–9. https://doi.org/10.1016/s0002-9440(10)62487-x.
Grommes C, DeAngelis LM. Primary CNS lymphoma. J Clin Oncol. 2017;35(21):2410–8. https://doi.org/10.1200/jco.2017.72.7602.
You H, Wei L, Kaminska B. Emerging insights into origin and pathobiology of primary central nervous system lymphoma. Cancer Lett. 2021;509:121–9. https://doi.org/10.1016/j.canlet.2021.02.025.
Yang H, Xun Y, Yang A, Liu F, You H. Advances and challenges in the treatment of primary central nervous system lymphoma. J Cell Physiol. 2020;235(12):9143–65. https://doi.org/10.1002/jcp.29790.
David KA, Sundaram S, Kim SH, Vaca R, Lin Y, Singer S, et al. Older patients with primary central nervous system lymphoma: Survival and prognostication across 20 U.S. cancer centers. Am J Hematol. 2023;98(6):900–12. https://doi.org/10.1002/ajh.26919.
Schrum DP, Moorman MT, Li Z, Dillon M, Peters KB, McKinney M et al. Comparison of differing dose levels of methotrexate for patients with primary central nervous system lymphoma. J Oncol Pharm Pract. 2023:10781552231176754. https://doi.org/10.1177/10781552231176754.
Villanueva G, Guscott M, Schaiquevich P, Sampor C, Combs R, Tentoni N, et al. A systematic review of high-dose methotrexate for adults with primary central nervous system lymphoma. Cancers (Basel). 2023;15(5):1459. https://doi.org/10.3390/cancers15051459.
Mishima K, Nishikawa R, Narita Y, Mizusawa J, Sumi M, Koga T, et al. Randomized phase III study of high-dose methotrexate and whole-brain radiotherapy with/without temozolomide for newly diagnosed primary CNS lymphoma: JCOG1114C. Neuro Oncol. 2023;25(4):687–98. https://doi.org/10.1093/neuonc/noac246.
Kaji FA, Martinez-Calle N, Bishton MJ, Figueroa R, Adlington J, O’Donoghue M, et al. Improved survival outcomes despite older age at diagnosis: an era-by-era analysis of patients with primary central nervous system lymphoma treated at a single referral centre in the United Kingdom. Br J Haematol. 2021;195(4):561–70. https://doi.org/10.1111/bjh.17747.
Sanders S, Chua N, Larouche JF, Owen C, Shafey M, Stewart DA. Outcomes of consecutively diagnosed primary central nervous system lymphoma patients using the Alberta lymphoma clinical practice guideline incorporating thiotepa-busulfan conditioning for transplantation-eligible patients. Biol Blood Marrow Transplant. 2019;25(8):1505–10. https://doi.org/10.1016/j.bbmt.2019.04.004.
Seidel S, Kowalski T, Margold M, Baraniskin A, Schroers R, Martus P, et al. HDMTX-based polychemotherapy including intraventricular therapy in elderly patients with primary CNS lymphoma: a single center series. Ther Adv Neurol Disord. 2020;13:1756286420951087. https://doi.org/10.1177/1756286420951087.
Seidel S, Margold M, Kowalski T, Baraniskin A, Schroers R, Korfel A, et al. Patients with primary central nervous system lymphoma not eligible for clinical trials: prognostic factors, treatment and outcome. Cancers (Basel). 2021;13(12):2934. https://doi.org/10.3390/cancers13122934.
Yerram P, Reiss SN, Modelevsky L, Schaff L, Reiner AS, Panageas KS, et al. Is more better? Increased doses of high dose methotrexate and addition of rituximab is associated with improved outcomes in a large primary CNS lymphoma cohort. Ann Lymphoma. 2023;7:1. https://doi.org/10.21037/aol-22-19.
Reni M, Ferreri AJM, Garancini MP, Villa E. Therapeutic management of primary central nervous system lymphoma in immunocompetent patients: Results of a critical review of the literature. Ann Oncol. 1997;8(3):227–34. https://doi.org/10.1023/a:1008201717089.
Abrey LE, Yahalom J, DeAngelis LM. Treatment for primary CNS lymphoma: the next step. J Clin Oncol. 2000;18(17):3144–50. https://doi.org/10.1200/JCO.2000.18.17.3144.
Deangelis LM, Seiferheld W, Schold SC, Fisher B, Schultz CJ. Combination chemotherapy and radiotherapy for primary central nervous system lymphoma: Radiation Therapy Oncology Group Study 93–10. J Clin Oncol. 2002;20(24):4643–8. https://doi.org/10.1200/JCO.2002.11.013.
Burton EC, Ugiliweneza B, Kolikonda MK, Saaraswat T, Woo S, Boakye M, et al. A regional multicenter retrospective analysis of patients with primary central nervous system lymphoma diagnosed from 2000–2012: treatment patterns and clinical outcomes. Cureus. 2017;9(7):e1512. https://doi.org/10.7759/cureus.1512.
Ferreri AJ, Reni M, Villa E. Therapeutic management of primary central nervous system lymphoma: lessons from prospective trials. Ann Oncol. 2000;11(8):927–37. https://doi.org/10.1023/a:1008376412784.
Milgrom SA, Yahalom J. The role of radiation therapy in the management of primary central nervous system lymphoma. Leuk Lymphoma. 2015;56(5):1197–204. https://doi.org/10.3109/10428194.2014.961014.
Chalise L, Motomura K, Ohka F, Hirano M, Hara M, Nishimura Y, et al. Comparing the efficacy of deVIC therapy and high-dose methotrexate monotherapy with whole-brain radiation therapy for newly-diagnosed primary central nervous system lymphoma: a single institution study. Anticancer Res. 2017;37(9):5215–23. https://doi.org/10.21873/anticanres.11945.
Chen T, Liu Y, Wang Y, Chang Q, Wu J, Wang Z, et al. Evidence-based expert consensus on the management of primary central nervous system lymphoma in China. J Hematol Oncol. 2022;15(1):136. https://doi.org/10.1186/s13045-022-01356-7.
Miyao K, Yokota H, Sakemura RL. Is CD19-directed chimeric antigen receptor T cell therapy a smart strategy to combat central nervous system lymphoma? Front Oncol. 2022;12:1082235. https://doi.org/10.3389/fonc.2022.1082235.
Mizushima M, Ishi Y, Ikeda H, Echizenya I, Otsuka T, Mitsuhashi T, et al. Successful treatment of intracranial methotrexate-associated lymphoproliferative disorder without Epstein-Barr virus infection using rituximab, methotrexate, procarbazine, and vincristine: a case report. NMC Case Rep J. 2022;9:237–42. https://doi.org/10.2176/jns-nmc.2022-0091.
Ostrowska B, Domanska-Czyz K, Romejko-Jarosinska J, Osowiecki M, Targonski L, Poplawska L, et al. Safety and efficacy of induction immunochemotherapy with rituximab, methotrexate, ifosfamide, and vincristine (R-MIV) in patients with primary CNS lymphoma including recent COVID-19 pandemic experience. Br J Haematol. 2023;201(4):663–72. https://doi.org/10.1111/bjh.18687.
Seidel S, Kowalski T, Nilius-Eliliwi V, Schroers R, Schlegel U. Survival, prognostic factors, hospitalization time and clinical performance status after first cerebral relapse or progression in 54 patients with primary CNS lymphoma not eligible for high dose chemotherapy: a retrospective analysis. Neurol Res Pract. 2023;5(1):8. https://doi.org/10.1186/s42466-023-00234-y.
Wendler J, Fox CP, Valk E, Steinheber C, Fricker H, Isbell LK, et al. Optimizing MATRix as remission induction in PCNSL: de-escalated induction treatment in newly diagnosed primary CNS lymphoma. BMC Cancer. 2022;22(1):971. https://doi.org/10.1186/s12885-022-09723-w.
Yuan X, Yu T, Huang Y, Jiang H, Xu X, Liang Y, et al. Rituximab with high-dose methotrexate is effective and cost-effective in newly diagnosed primary central nervous system lymphoma. Sci Rep. 2022;12(1):21541. https://doi.org/10.1038/s41598-022-24922-y.
Brugnoletti F, Morris EB, Laningham FH, Patay Z, Pauley JL, Pui CH, et al. Recurrent intrathecal methotrexate induced neurotoxicity in an adolescent with acute lymphoblastic leukemia: Serial clinical and radiologic findings. Pediatr Blood Cancer. 2009;52(2):293–5. https://doi.org/10.1002/pbc.21764.
Schorb E, Kasenda B, Atta J, Kaun S, Morgner A, Hess G, et al. Prognosis of patients with primary central nervous system lymphoma after high-dose chemotherapy followed by autologous stem cell transplantation. Haematologica. 2013;98(5):765–70. https://doi.org/10.3324/haematol.2012.076075.
Omuro A, Correa DD, DeAngelis LM, Moskowitz CH, Matasar MJ, Kaley TJ, et al. R-MPV followed by high-dose chemotherapy with TBC and autologous stem-cell transplant for newly diagnosed primary CNS lymphoma. Blood. 2015;125(9):1403–10. https://doi.org/10.1182/blood-2014-10-604561.
Illerhaus G, Kasenda B, Ihorst G, Egerer G, Lamprecht M, Keller U, et al. High-dose chemotherapy with autologous haemopoietic stem cell transplantation for newly diagnosed primary CNS lymphoma: a prospective, single-arm, phase 2 trial. Lancet Haematol. 2016;3(8):e388–97. https://doi.org/10.1016/S2352-3026(16)30050-3.
Ferreri AJM, Cwynarski K, Pulczynski E, Fox CP, Schorb E, La Rosée P, et al. Whole-brain radiotherapy or autologous stem-cell transplantation as consolidation strategies after high-dose methotrexate-based chemoimmunotherapy in patients with primary CNS lymphoma: results of the second randomisation of the International Extranodal Lymphoma Study Group-32 phase 2 trial. Lancet Haematol. 2017;4(11):e510–23. https://doi.org/10.1016/S2352-3026(17)30174-6.
Nakasu Y, Mitsuya K, Hayashi N, Okamura I, Mori K, Enami T, et al. Response-adapted treatment with upfront high-dose chemotherapy followed by autologous stem-cell transplantation rescue or consolidation phase high-dose methotrexate for primary central nervous system lymphoma: a long-term mono-center study. Springerplus. 2016;5(1):307. https://doi.org/10.1186/s40064-016-1954-6.
Bojic M, Berghoff AS, Troch M, Agis H, Sperr WR, Widhalm G, et al. Haematopoietic stem cell transplantation for treatment of primary CNS lymphoma: Single centre experience and literature review. Eur J Haematol. 2015;95(1):75–82. https://doi.org/10.1111/ejh.12482.
Kuitunen H, Tokola S, Siniluoto T, Isokangas M, Sonkajärvi E, Alahuhta S, et al. Promising treatment results with blood brain barrier disruption (BBBD) based immunochemotherapy combined with autologous stem cell transplantation (ASCT) in patients with primary central nervous system lymphoma (PCNSL). J Neurooncol. 2017;131(2):1–8. https://doi.org/10.1007/s11060-016-2293-8.
Soussain C, Hoang-Xuan K, Taillandier L, Fourme E, Choquet S, Witz F, et al. Intensive chemotherapy followed by hematopoietic stem-cell rescue for refractory and recurrent primary CNS and intraocular lymphoma: Société Française de Greffe de Moëlle Osseuse-Thérapie Cellulaire. J Clin Oncol. 2008;26(15):2512–8. https://doi.org/10.1200/jco.2007.13.5533.
Soussain C, Suzan F, Hoang-Xuan K, Cassoux N, Levy V, Azar N, et al. Results of intensive chemotherapy followed by hematopoietic stem-cell rescue in 22 patients with refractory or recurrent primary CNS lymphoma or intraocular lymphoma. J Clin Oncol. 2001;19(3):742–9. https://doi.org/10.1200/jco.2001.19.3.742.
Dholaria BR, Kumar A, Azzuqua AG, Nishihori T, Kharfan-Dabaja MA, Tun HW, et al. Autologous stem cell transplantation in central nervous system lymphoma: a multicenter retrospective series and a review of the literature. Clin Lymphoma Myeloma Leuk. 2019;19(6):e273–80. https://doi.org/10.1016/j.clml.2019.02.013.
Lionakis MS, Dunleavy K, Roschewski M, Widemann BC, Butman JA, Schmitz R, et al. Inhibition of B cell receptor signaling by ibrutinib in primary CNS lymphoma. Cancer Cell. 2017;31(6):833-43.e5. https://doi.org/10.1016/j.ccell.2017.04.012.
Feng L, Gao X, Jiao Z, Wang Z, Min F. BTK inhibitor combined with anti-PD-1 monoclonal antibody for the treatment of CD20-negative primary central nervous system lymphoma: a case report. Oncol Lett. 2023;25(2):48. https://doi.org/10.3892/ol.2022.13634.
Nepal G, Khurana M, Bucheli DH, Bhandari S, Joshi U, Bhagat R, et al. Ibrutinib in refractory or relapsing primary central nervous system lymphoma: a systematic review. Neurol Int. 2022;14(1):99–108. https://doi.org/10.3390/neurolint14010009.
Okita Y, Kano-Fujiwara R, Nakatsuka SI, Honma K, Kinoshita M. Histological verification of the treatment effect of tirabrutinib for relapsed/refractory primary central nervous system lymphoma. Exp Hematol Oncol. 2021;10(1):29. https://doi.org/10.1186/s40164-021-00222-5.
Rachdi A, Hernandez-Tost H, Herzi D, Morales-Martinez A, Hernández-Verdin I, Houillier C, et al. Recent advances in the diagnosis and the treatment of primary CNS lymphoma. Rev Neurol (Paris). 2023;179(5):481–9. https://doi.org/10.1016/j.neurol.2023.03.012.
Wang S, Zhu Y, Qian X, Ding T, Yuan Y, Li Y et al. The outcome of ibrutinib-based regimens in relapsed/refractory central nervous system lymphoma and the potential impact of genomic variants. Adv Clin Exp Med. 2023. https://doi.org/10.17219/acem/159288.
Yang C, Cui Y, Ren X, Li M, Yu K, Shen S, et al. Orelabrutinib combined with lenalidomide and immunochemotherapy for relapsed/refractory primary central nervous system lymphoma: a retrospective analysis of case series. Front Oncol. 2022;12:901797. https://doi.org/10.3389/fonc.2022.901797.
Yu H, Kong H, Li C, Dong X, Wu Y, Zhuang Y, et al. Bruton’s tyrosine kinase inhibitors in primary central nervous system lymphoma-evaluation of anti-tumor efficacy and brain distribution. Transl Cancer Res. 2021;10(5):1975–83. https://doi.org/10.21037/tcr-21-50.
Liu Y, Sun J, Tuo K. Zanubrutinib in the maintenance treatment of elderly people with primary central nervous system lymphoma: a report of 2 cases. Case Rep Oncol. 2023;16(1):227–33. https://doi.org/10.1159/000529315.
Chamoun K, Choquet S, Boyle E, Houillier C, Larrieu-Ciron D, Al Jijakli A, et al. Ibrutinib monotherapy in relapsed/refractory CNS lymphoma: a retrospective case series. Neurology. 2017;88(1):101–2. https://doi.org/10.1212/wnl.0000000000003420.
Alcantara M, Houillier C, Blonski M, Rubio MT, Willems L, Rascalou AW, et al. CAR T-cell therapy in primary central nervous system lymphoma: the clinical experience of the French LOC network. Blood. 2022;139(5):792–6. https://doi.org/10.1182/blood.2021012932.
Frigault MJ, Dietrich J, Martinez-Lage M, Leick M, Choi BD, DeFilipp Z, et al. Tisagenlecleucel CAR T-cell therapy in secondary CNS lymphoma. Blood. 2019;134(11):860–6. https://doi.org/10.1182/blood.2019001694.
Abramson JS, McGree B, Noyes S, Plummer S, Wong C, Chen YB, et al. Anti-CD19 CAR T cells in CNS diffuse large B-cell lymphoma. N Engl J Med. 2017;377(8):783–4. https://doi.org/10.1056/NEJMc1704610.
Hayabuchi N, Shibamoto Y, Onizuka Y. Primary central nervous system lymphoma in Japan: a nationwide survey. Int J Radiat Oncol Biol Phys. 1999;44(2):265–72. https://doi.org/10.1016/s0360-3016(98)00564-1.
Niparuck P, Boonsakan P, Sutthippingkiat T, Pukiat S, Chantrathammachart P, Phusanti S, et al. Treatment outcome and prognostic factors in PCNSL. Diagn Pathol. 2019;14(1):56. https://doi.org/10.1186/s13000-019-0833-1.
Liu CJ, Lin SY, Yang CF, Yeh CM, Kuan AS, Wang HY, et al. A new prognostic score for disease progression and mortality in patients with newly diagnosed primary CNS lymphoma. Cancer Med. 2020;9(6):2134–45. https://doi.org/10.1002/cam4.2872.
Ouyang T, Wang L, Zhang N, Zhang Z, Xiong Y, Li M, et al. Clinical characteristics, surgical outcomes, and prognostic factors of intracranial primary central nervous system lymphoma. World Neurosurg. 2020;139:e508–16. https://doi.org/10.1016/j.wneu.2020.04.049.
Ferreri AJ, Blay JY, Reni M, Pasini F, Spina M, Ambrosetti A, et al. Prognostic scoring system for primary CNS lymphomas: the International Extranodal Lymphoma Study Group experience. J Clin Oncol. 2003;21(2):266–72. https://doi.org/10.1200/jco.2003.09.139.
Jahr G, Broi MD, Holte H Jr, Beiske K, Meling TR. Evaluation of Memorial Sloan-Kettering Cancer Center and International Extranodal Lymphoma Study Group prognostic scoring systems to predict overall survival in intracranial primary CNS lymphoma. Brain Behav. 2018;8(3):e00928. https://doi.org/10.1002/brb3.928.
Ghesquières H, Drouet Y, Sunyach MP, Sebban C, Chassagne-Clement C, Jouanneau E, et al. Evidence of time-dependent prognostic factors predicting early death but not long-term outcome in primary CNS lymphoma: a study of 91 patients. Hematol Oncol. 2013;31(2):57–64. https://doi.org/10.1002/hon.2021.
Borba EA, Scoto Dias E, Tercziany Vanzin JH, Ferreira de Queiroz Junior N, Dos Santos TAF, Skare T et al. Cognitive dysfunction in patients with systemic lupus erythematosus. A cross-sectional study in a Brazilian sample. Lupus. 2023:9612033231176794. https://doi.org/10.1177/09612033231176794.
Carranza-Lira S, Jimeno BLM, Ortiz SR. The relationship between carotid intima-media thickness and cognitive function and depression in postmenopausal women. Prz Menopauzalny. 2023;22(1):21–3. https://doi.org/10.5114/pm.2023.126363.
Park J, Lee HJ, Park JS, Kim CH, Jung WJ, Won S, et al. Development of a gait feature-based model for classifying cognitive disorders using a single wearable inertial sensor. Neurology. 2023. https://doi.org/10.1212/wnl.0000000000207372.
Zhou W, Xie X, Hu J, Wang M, Hu X, Shi L, et al. Relationship between microstructural alterations and cognitive decline after whole-brain radiation therapy for brain metastases: an exploratory whole-brain MR analysis based on neurite orientation dispersion and density imaging. J Magn Reson Imaging. 2023. https://doi.org/10.1002/jmri.28781.
Klein M, Postma TJ, Taphoorn MJ, Aaronson NK, Vandertop WP, Muller M, et al. The prognostic value of cognitive functioning in the survival of patients with high-grade glioma. Neurology. 2003;61(12):1796–8. https://doi.org/10.1212/01.wnl.0000098892.33018.4c.
Daniels TB, Brown PD, Felten SJ, Wu W, Buckner JC, Arusell RM, et al. Validation of EORTC prognostic factors for adults with low-grade glioma: a report using intergroup 86–72-51. Int J Radiat Oncol Biol Phys. 2011;81(1):218–24. https://doi.org/10.1016/j.ijrobp.2010.05.003.
van der Meulen M, Dirven L, Bakunina K, van den Bent MJ, Issa S, Doorduijn JK, et al. MMSE is an independent prognostic factor for survival in primary central nervous system lymphoma. J Neurooncol. 2021;152(2):357–62. https://doi.org/10.1007/s11060-021-03708-8.
Kreher S, Johrens K, Strehlow F, Martus P, Borowiec K, Radke J, et al. Prognostic impact of B-cell lymphoma 6 in primary CNS lymphoma. Neuro Oncol. 2015;17(7):1016–21. https://doi.org/10.1093/neuonc/nov046.
Patel B, Chacko G, Nair S, Anandan J, Chacko AG, Rajshekhar V, et al. Clinicopathological correlates of primary central nervous system lymphoma: experience from a tertiary care center in South India. Neurol India. 2015;63(1):77–82. https://doi.org/10.4103/0028-3886.152658.
Lee J, Shishido-Hara Y, Suzuki K, Shimizu S, Kobayashi K, Kamma H, et al. Prognostic factors for primary central nervous system lymphomas treated with high-dose methotrexate-based chemo-radiotherapy. Jpn J Clin Oncol. 2017;47(10):925–34. https://doi.org/10.1093/jjco/hyx098.
Radotra BD, Parkhi M, Chatterjee D, Yadav BS, Ballari NR, Prakash G, et al. Clinicopathological features of primary central nervous system diffuse large B cell lymphoma: experience from a tertiary center in North India. Surg Neurol Int. 2020;11:424. https://doi.org/10.25259/sni_314_2020.
Lin CH, Kuo KT, Chuang SS, Kuo SH, Chang JH, Chang KC, et al. Comparison of the expression and prognostic significance of differentiation markers between diffuse large B-cell lymphoma of central nervous system origin and peripheral nodal origin. Clin Cancer Res. 2006;12(4):1152–6. https://doi.org/10.1158/1078-0432.Ccr-05-1699.
Marcus C, Maragkos GA, Alterman RL, Uhlmann E, Pihan G, Varma H. GCB-type is a favorable prognostic factor in primary CNS diffuse large B-cell lymphomas. J Clin Neurosci. 2021;83:49–55. https://doi.org/10.1016/j.jocn.2020.11.031.
Tang D, Su W, Wang X, Chu Z, Zhang L, Zhou J, et al. Clinicopathologic significance of MYD88 L265P mutation and expression of TLR4 and P-STAT3 in primary central nervous system diffuse large B-cell lymphomas. Brain Tumor Pathol. 2021;38(1):50–8. https://doi.org/10.1007/s10014-020-00386-8.
Cho U, Oh WJ, Hong YK, Lee YS. Prognostic significance of high Ki-67 index and histogenetic subclassification in primary central nervous system lymphoma. Appl Immunohistochem Mol Morphol. 2018;26(4):254–62. https://doi.org/10.1097/pai.0000000000000424.
Friedberg JW. How I treat double-hit lymphoma. Blood. 2017;130(5):590–6. https://doi.org/10.1182/blood-2017-04-737320.
Li W, Gupta SK, Han W, Kundson RA, Nelson S, Knutson D, et al. Targeting MYC activity in double-hit lymphoma with MYC and BCL2 and/or BCL6 rearrangements with epigenetic bromodomain inhibitors. J Hematol Oncol. 2019;12(1):73. https://doi.org/10.1186/s13045-019-0761-2.
Riedell PA, Smith SM. Double hit and double expressors in lymphoma: definition and treatment. Cancer. 2018;124(24):4622–32. https://doi.org/10.1002/cncr.31646.
Rosenthal A, Younes A. High grade B-cell lymphoma with rearrangements of MYC and BCL2 and/or BCL6: double hit and triple hit lymphomas and double expressing lymphoma. Blood Rev. 2017;31(2):37–42. https://doi.org/10.1016/j.blre.2016.09.004.
Xu-Monette ZY, Wei L, Fang X, Au Q, Nunns H, Nagy M, et al. Genetic subtyping and phenotypic characterization of the immune microenvironment and MYC/BCL2 double expression reveal heterogeneity in diffuse large B-cell lymphoma. Clin Cancer Res. 2022;28(5):972–83. https://doi.org/10.1158/1078-0432.Ccr-21-2949.
Ganapathi KA, Brown LE, Prakash S, Bhargava P. New developments in non-Hodgkin lymphoid malignancies. Pathology. 2021;53(3):349–66. https://doi.org/10.1016/j.pathol.2021.01.002.
Kawashima I, Inamoto Y, Maeshima AM, Nomoto J, Tajima K, Honda T, et al. Double-expressor lymphoma is associated with poor outcomes after allogeneic hematopoietic cell transplantation. Biol Blood Marrow Transplant. 2018;24(2):294–300. https://doi.org/10.1016/j.bbmt.2017.10.013.
Reagan PM, Davies A. Current treatment of double hit and double expressor lymphoma. Hematology Am Soc Hematol Educ Program. 2017;2017(1):295–7. https://doi.org/10.1182/asheducation-2017.1.295.
Hu S, Xu-Monette ZY, Tzankov A, Green T, Wu L, Balasubramanyam A, et al. MYC/BCL2 protein coexpression contributes to the inferior survival of activated B-cell subtype of diffuse large B-cell lymphoma and demonstrates high-risk gene expression signatures: a report from The International DLBCL Rituximab-CHOP Consortium Program. Blood. 2013;121(20):4021–31. https://doi.org/10.1182/blood-2012-10-460063. quiz 250.
Liu G, Zhang X, Zhang N, Xiao H, Chen X, Ma L. Detecting double expression status in primary central nervous system lymphoma using multiparametric MRI based machine learning. J Magn Reson Imaging. 2023. https://doi.org/10.1002/jmri.28782.
Nosrati A, Monabati A, Sadeghipour A, Radmanesh F, Safaei A, Movahedinia S. MYC, BCL2, and BCL6 rearrangements in primary central nervous system lymphoma of large B cell type. Ann Hematol. 2019;98(1):169–73. https://doi.org/10.1007/s00277-018-3498-z.
Hatzl S, Posch F, Deutsch A, Beham-Schmid C, Stöger H, Greinix H, et al. Immunohistochemistry for c-myc and bcl-2 overexpression improves risk stratification in primary central nervous system lymphoma. Hematol Oncol. 2020;38(3):277–83. https://doi.org/10.1002/hon.2727.
Asano K, Yamashita Y, Ono T, Natsumeda M, Beppu T, Matsuda K, et al. Clinicopathological risk factors for a poor prognosis of primary central nervous system lymphoma in elderly patients in the Tohoku and Niigata area: a multicenter, retrospective, cohort study of the Tohoku Brain Tumor Study Group. Brain Tumor Pathol. 2022;39(3):139–50. https://doi.org/10.1007/s10014-022-00427-4.
Ge L, Lu S, Xu L, Yan H. MYC, BCL2, and BCL6 expression as prognostic indicators in primary central nervous system lymphoma: a systematic review and meta-analysis. Clin Neurol Neurosurg. 2021;208:106838. https://doi.org/10.1016/j.clineuro.2021.106838.
Furtner J, Nenning KH. Evaluation of the temporal muscle thickness as an independent prognostic biomarker in patients with primary central nervous system lymphoma. Cancers (Basel). 2021;13(3):566. https://doi.org/10.3390/cancers13030566.
Leone R, Sferruzza G, Calimeri T, Steffanoni S, Conte GM, De Cobelli F, et al. Quantitative muscle mass biomarkers are independent prognosis factors in primary central nervous system lymphoma: The role of L3-skeletal muscle index and temporal muscle thickness. Eur J Radiol. 2021;143:109945. https://doi.org/10.1016/j.ejrad.2021.109945.
Barajas RF Jr, Rubenstein JL, Chang JS, Hwang J, Cha S. Diffusion-weighted MR imaging derived apparent diffusion coefficient is predictive of clinical outcome in primary central nervous system lymphoma. AJNR Am J Neuroradiol. 2010;31(1):60–6. https://doi.org/10.3174/ajnr.A1750.
Valles FE, Perez-Valles CL, Regalado S, Barajas RF, Rubenstein JL, Cha S. Combined diffusion and perfusion MR imaging as biomarkers of prognosis in immunocompetent patients with primary central nervous system lymphoma. AJNR Am J Neuroradiol. 2013;34(1):35–40. https://doi.org/10.3174/ajnr.A3165.
Zhang Y, Zhang Q, Wang XX, Deng XF, Zhu YZ. Value of pretherapeutic DWI in evaluating prognosis and therapeutic effect in immunocompetent patients with primary central nervous system lymphoma given high-dose methotrexate-based chemotherapy: ADC-based assessment. Clin Radiol. 2016;71(10):1018–29. https://doi.org/10.1016/j.crad.2016.05.017.
Baek DW, Cho HJ, Bae JH, Sohn SK, Moon JH. Apparent diffusion coefficient as a valuable quantitative parameter for predicting clinical outcomes in patients with newly diagnosed primary CNS lymphoma. Blood Res. 2020;55(2):99–106. https://doi.org/10.5045/br.2020.2020032.
Palmedo H, Urbach H, Bender H, Schlegel U, Schmidt-Wolf IG, Matthies A, et al. FDG-PET in immunocompetent patients with primary central nervous system lymphoma: correlation with MRI and clinical follow-up. Eur J Nucl Med Mol Imaging. 2006;33(2):164–8. https://doi.org/10.1007/s00259-005-1917-6.
Gupta M, Gupta T, Purandare N, Rangarajan V, Puranik A, Moiyadi A, et al. Utility of flouro-deoxy-glucose positron emission tomography/computed tomography in the diagnostic and staging evaluation of patients with primary CNS lymphoma. CNS Oncol. 2019;8(4):Cns46. https://doi.org/10.2217/cns-2019-0016.
Yi C, Shi X, Yu D, Luo G, Zhang B, He Q, et al. The combination of 13N-ammonia and 18F-FDG PET/CT in the identification of metabolic phenotype of primary human brain tumors. Nuklearmedizin. 2019;58(3):272–8. https://doi.org/10.1055/a-0835-5746.
Cui C, Yao X, Xu L, Chao Y, Hu Y, Zhao S, et al. Improving the classification of PCNSL and brain metastases by developing a machine learning model based on (18)F-FDG PET. J Pers Med. 2023;13(3):539. https://doi.org/10.3390/jpm13030539.
Uchinomura S, Mitamura K, Norikane T, Yamamoto Y, Oishi A, Hatakeyama T, et al. Distinguishing between primary central nervous system lymphoma and glioblastoma using [18F]fluoromisonidazole and [18F]FDG PET. Nucl Med Commun. 2022;43(3):270–4. https://doi.org/10.1097/mnm.0000000000001510.
Zhou W, Wen J, Hua F, Xu W, Lu X, Yin B, et al. (18)F-FDG PET/CT in immunocompetent patients with primary central nervous system lymphoma: differentiation from glioblastoma and correlation with DWI. Eur J Radiol. 2018;104:26–32. https://doi.org/10.1016/j.ejrad.2018.04.020.
Mohile NA, Deangelis LM, Abrey LE. The utility of body FDG PET in staging primary central nervous system lymphoma. Neuro Oncol. 2008;10(2):223–8. https://doi.org/10.1215/15228517-2007-061.
Gupta T, Manjali JJ, Kannan S, Purandare N, Rangarajan V. Diagnostic yield of extensive systemic staging including whole-body 18F-fluoro-deoxy-glucose positron emission tomography with or without computed tomography in patients with primary central nervous system lymphoma: systematic review and meta-analysis. Clin Lymphoma Myeloma Leuk. 2020;20(11):e836–45. https://doi.org/10.1016/j.clml.2020.06.019.
Kawai N, Zhen HN, Miyake K, Yamamaoto Y, Nishiyama Y, Tamiya T. Prognostic value of pretreatment 18F-FDG PET in patients with primary central nervous system lymphoma: SUV-based assessment. J Neurooncol. 2010;100(2):225–32. https://doi.org/10.1007/s11060-010-0182-0.
Ferreri AJ, Reni M. Prognostic factors in primary central nervous system lymphomas. Hematol Oncol Clin North Am. 2005;19(4):629–494, vi. https://doi.org/10.1016/j.hoc.2005.05.005.
Blay JY, Bouhour D, Carrie C, Bouffet E, Brunat-Mentigny M, Philip T, et al. The C5R protocol: a regimen of high-dose chemotherapy and radiotherapy in primary cerebral non-Hodgkin’s lymphoma of patients with no known cause of immunosuppression. Blood. 1995;86(8):2922–9. https://doi.org/10.1182/blood.V86.8.2922.2922.
Sun X, Wang C, Chen C, Huang J, Wu X, Wang Y, et al. Combined tumor-associated macrophages biomarker predicting extremely poor outcome of patients with primary central nervous system lymphoma. Hematol Oncol. 2021;39(5):625–38. https://doi.org/10.1002/hon.2926.
Bessell EM, Graus F, Lopez-Guillermo A, Lewis SA, Villa S, Verger E, et al. Primary non-Hodgkin’s lymphoma of the CNS treated with CHOD/BVAM or BVAM chemotherapy before radiotherapy: long-term survival and prognostic factors. Int J Radiat Oncol Biol Phys. 2004;59(2):501–8. https://doi.org/10.1016/j.ijrobp.2003.11.001.
Abrey LE, Ben-Porat L, Panageas KS, Yahalom J, Berkey B, Curran W, et al. Primary central nervous system lymphoma: the Memorial Sloan-Kettering Cancer Center prognostic model. J Clin Oncol. 2006;24(36):5711–5. https://doi.org/10.1200/jco.2006.08.2941.
Gao Y, Wei L, Kim SJ, Wang L, He Y, Zheng Y, et al. A novel prognostic marker for primary CNS lymphoma: lactate dehydrogenase-to-lymphocyte ratio improves stratification of patients within the low and intermediate MSKCC risk groups. Front Oncol. 2021;11:696147. https://doi.org/10.3389/fonc.2021.696147.
Le M, Garcilazo Y, Ibáñez-Juliá MJ, Younan N, Royer-Perron L, Benazra M, et al. Pretreatment hemoglobin as an independent prognostic factor in primary central nervous system lymphomas. Oncologist. 2019;24(9):e898–904. https://doi.org/10.1634/theoncologist.2018-0629.
Jang JE, Kim YR, Kim SJ, Cho H, Chung H, Lee JY, et al. A new prognostic model using absolute lymphocyte count in patients with primary central nervous system lymphoma. Eur J Cancer. 2016;57:127–35. https://doi.org/10.1016/j.ejca.2016.01.016.
Jung J, Lee H, Yun T, Lee E, Moon H, Joo J, et al. Prognostic role of the neutrophil-to-lymphocyte ratio in patients with primary central nervous system lymphoma. Oncotarget. 2017;8(43):74975–86. https://doi.org/10.18632/oncotarget.20480.
Luo Q, Yang C, Fu C, Wu W, Wei Y, Zou L. Prognostic role of blood markers in primary central nervous system lymphoma patients treated with high-dose methotrexate-based therapy. Front Oncol. 2021;11:639644. https://doi.org/10.3389/fonc.2021.639644.
Yoong Y, Porrata LF, Inwards DJ, Ansell SM, Micallef IN, Litzow MR, et al. The effect of absolute lymphocyte count recovery kinetics on survival after autologous stem cell transplantation for non-Hodgkin’s lymphoma. Leuk Lymphoma. 2005;46(9):1287–94. https://doi.org/10.1080/10428190500126380.
Porrata LF, Litzow MR, Inwards DJ, Gastineau DA, Moore SB, Pineda AA, et al. Infused peripheral blood autograft absolute lymphocyte count correlates with day 15 absolute lymphocyte count and clinical outcome after autologous peripheral hematopoietic stem cell transplantation in non-Hodgkin’s lymphoma. Bone Marrow Transplant. 2004;33(3):291–8. https://doi.org/10.1038/sj.bmt.1704355.
Yoon DH, Sohn BS, Jang G, Kim EK, Kang BW, Kim C, et al. Higher infused CD34+ hematopoietic stem cell dose correlates with earlier lymphocyte recovery and better clinical outcome after autologous stem cell transplantation in non-Hodgkin’s lymphoma. Transfusion. 2009;49(9):1890–900. https://doi.org/10.1111/j.1537-2995.2009.02202.x.
Coussens LM, Werb Z. Inflammation and cancer. Nature. 2002;420(6917):860–7. https://doi.org/10.1038/nature01322.
Berraondo P, Sanmamed MF, Ochoa MC, Etxeberria I, Aznar MA, Pérez-Gracia JL, et al. Cytokines in clinical cancer immunotherapy. Br J Cancer. 2019;120(1):6–15. https://doi.org/10.1038/s41416-018-0328-y.
Ciaraldi TP, Aroda V, Mudaliar SR, Henry RR. Inflammatory cytokines and chemokines, skeletal muscle and polycystic ovary syndrome: effects of pioglitazone and metformin treatment. Metabolism. 2013;62(11):1587–96. https://doi.org/10.1016/j.metabol.2013.07.004.
Lippitz BE. Cytokine patterns in patients with cancer: a systematic review. Lancet Oncol. 2013;14(6):e218–28. https://doi.org/10.1016/s1470-2045(12)70582-x.
Propper DJ, Balkwill FR. Harnessing cytokines and chemokines for cancer therapy. Nat Rev Clin Oncol. 2022;19(4):237–53. https://doi.org/10.1038/s41571-021-00588-9.
Salazar-Onfray F, López MN, Mendoza-Naranjo A. Paradoxical effects of cytokines in tumor immune surveillance and tumor immune escape. Cytokine Growth Factor Rev. 2007;18(1–2):171–82. https://doi.org/10.1016/j.cytogfr.2007.01.015.
Smyth MJ, Cretney E, Kershaw MH, Hayakawa Y. Cytokines in cancer immunity and immunotherapy. Immunol Rev. 2004;202:275–93. https://doi.org/10.1111/j.0105-2896.2004.00199.x.
Tartour E, Fridman WH. Cytokines and cancer. Int Rev Immunol. 1998;16(5–6):683–704. https://doi.org/10.3109/08830189809043014.
Van Gorp H, Lamkanfi M. The emerging roles of inflammasome-dependent cytokines in cancer development. EMBO Rep. 2019;20(6):e47575. https://doi.org/10.15252/embr.201847575.
Van Meir EG. Cytokines and tumors of the central nervous system. Glia. 1995;15(3):264–88. https://doi.org/10.1002/glia.440150308.
Wieder T, Brenner E, Braumüller H, Bischof O, Röcken M. Cytokine-induced senescence for cancer surveillance. Cancer Metastasis Rev. 2017;36(2):357–65. https://doi.org/10.1007/s10555-017-9667-z.
Diakos CI, Charles KA, McMillan DC, Clarke SJ. Cancer-related inflammation and treatment effectiveness. Lancet Oncol. 2014;15(11):e493-503. https://doi.org/10.1016/s1470-2045(14)70263-3.
Wang S, Ma Y, Sun L, Shi Y, Jiang S, Yu K, et al. Prognostic significance of pretreatment neutrophil/lymphocyte ratio and platelet/lymphocyte ratio in patients with diffuse large B-cell lymphoma. Biomed Res Int. 2018;2018:9651254. https://doi.org/10.1155/2018/9651254.
Annibali O, Hohaus S, Marchesi F, Cantonetti M, Di Rocco A, Tomarchio V, et al. The neutrophil/lymphocyte ratio ≥3.5 is a prognostic marker in diffuse large B-cell lymphoma: a retrospective analysis from the database of the Italian regional network “Rete Ematologica del Lazio per i Linfomi” (RELLI). Leuk Lymphoma. 2019;60(14):3386–94. https://doi.org/10.1080/10428194.2019.1633628.
Lo YT, Lim VY, Ng M, Tan YH, Chiang J, Chang EWY, et al. A prognostic model using post-steroid neutrophil-lymphocyte ratio predicts overall survival in primary central nervous system lymphoma. Cancers (Basel). 2022;14(7):1818. https://doi.org/10.3390/cancers14071818.
Dai W, Jia B, Yang J, Zhou S, Liu P, He X, et al. Development of new prognostic model based on pretreatment βLRI and LLRI for stage IE/IIE upper aerodigestive tract ENKTL, nasal type. Oncotarget. 2017;8(21):34787–95. https://doi.org/10.18632/oncotarget.16720.
Keane C, Tobin J, Talaulikar D, Green M, Crooks P, Jain S, et al. A high LDH to absolute lymphocyte count ratio in patients with DLBCL predicts for a poor intratumoral immune response and inferior survival. Oncotarget. 2018;9(34):23620–7. https://doi.org/10.18632/oncotarget.25306.
Wu XB, Hou SL, Liu H. Systemic immune inflammation index, ratio of lymphocytes to monocytes, lactate dehydrogenase and prognosis of diffuse large B-cell lymphoma patients. World J Clin Cases. 2021;9(32):9825–34. https://doi.org/10.12998/wjcc.v9.i32.9825.
Li T, Li H, Xie S, Tan Y, Xie ZP, Li WY, et al. Lactate dehydrogenase-to-lymphocyte ratio represents a powerful prognostic tool of metastatic renal cell carcinoma patients treated with tyrosine kinase inhibitors. Pathol Oncol Res. 2020;26(2):1319–24. https://doi.org/10.1007/s12253-019-00707-z.
Bokemeyer C, Oechsle K, Hartmann JT. Anaemia in cancer patients: pathophysiology, incidence and treatment. Eur J Clin Invest. 2005;35(Suppl 3):26–31. https://doi.org/10.1111/j.1365-2362.2005.01527.x.
Moncur A, Chowdhary M, Chu Y, Francis NK. Impact and outcomes of postoperative anaemia in colorectal cancer patients: a systematic review. Colorectal Dis. 2021;23(4):776–86. https://doi.org/10.1111/codi.15461.
Owusu C, Cohen HJ, Feng T, Tew W, Mohile SG, Klepin HD, et al. Anemia and functional disability in older adults with cancer. J Natl Compr Canc Netw. 2015;13(10):1233–9. https://doi.org/10.6004/jnccn.2015.0152.
Steinberg D. Anemia and cancer. CA Cancer J Clin. 1989;39(5):296–304. https://doi.org/10.3322/canjclin.39.5.296.
Bonavita E, Bromley CP, Jonsson G, Pelly VS, Sahoo S, Walwyn-Brown K, et al. Antagonistic inflammatory phenotypes dictate tumor fate and response to immune checkpoint blockade. Immunity. 2020;53(6):1215-29.e8. https://doi.org/10.1016/j.immuni.2020.10.020.
Bottazzi B, Riboli E, Mantovani A. Aging, inflammation and cancer. Semin Immunol. 2018;40:74–82. https://doi.org/10.1016/j.smim.2018.10.011.
Budisan L, Zanoaga O, Braicu C, Pirlog R, Covaliu B, Esanu V, et al. Links between infections, lung cancer, and the immune system. Int J Mol Sci. 2021;22(17):9394. https://doi.org/10.3390/ijms22179394.
Crusz SM, Balkwill FR. Inflammation and cancer: advances and new agents. Nat Rev Clin Oncol. 2015;12(10):584–96. https://doi.org/10.1038/nrclinonc.2015.105.
Hosseini F, Mahdian-Shakib A, Jadidi-Niaragh F, Enderami SE, Mohammadi H, Hemmatzadeh M, et al. Anti-inflammatory and anti-tumor effects of α-l-guluronic acid (G2013) on cancer-related inflammation in a murine breast cancer model. Biomed Pharmacother. 2018;98:793–800. https://doi.org/10.1016/j.biopha.2017.12.111.
Mantovani A, Allavena P, Sica A, Balkwill F. Cancer-related inflammation. Nature. 2008;454(7203):436–44. https://doi.org/10.1038/nature07205.
McDowell SAC, Quail DF. Immunological regulation of vascular inflammation during cancer metastasis. Front Immunol. 2019;10:1984. https://doi.org/10.3389/fimmu.2019.01984.
Parada-Cruz B, Aztatzi-Aguilar OG, Ramírez-Martínez G, Jacobo-Estrada TL, Cárdenas-González M, Escamilla-Rivera V, et al. Inflammation- and cancer-related microRNAs in rat renal cortex after subchronic exposure to fluoride. Chem Biol Interact. 2023;379:110519. https://doi.org/10.1016/j.cbi.2023.110519.
Raposo TP, Beirão BC, Pang LY, Queiroga FL, Argyle DJ. Inflammation and cancer: till death tears them apart. Vet J. 2015;205(2):161–74. https://doi.org/10.1016/j.tvjl.2015.04.015.
Shinko D, Diakos CI, Clarke SJ, Charles KA. Cancer-related systemic inflammation: the challenges and therapeutic opportunities for personalized medicine. Clin Pharmacol Ther. 2017;102(4):599–610. https://doi.org/10.1002/cpt.789.
Zengin M, Karahan İ. The role of cancer-related inflammation for prediction of poor survival in postmenopausal female patients with stage II/III colon cancer. Int Immunopharmacol. 2020;85:106624. https://doi.org/10.1016/j.intimp.2020.106624.
Tan KM, Chia B, Lim JQ, Khoo LP, Cheng CL, Tan L, et al. A clinicohaematological prognostic model for nasal-type natural killer/T-cell lymphoma: a multicenter study. Sci Rep. 2019;9(1):14961. https://doi.org/10.1038/s41598-019-51522-0.
Zhu JW, Charkhchi P, Akbari MR. Potential clinical utility of liquid biopsies in ovarian cancer. Mol Cancer. 2022;21(1):114. https://doi.org/10.1186/s12943-022-01588-8.
Zhu L, Zhao L, Wang Q, Zhong S, Guo X, Zhu Y, et al. Circulating exosomal miRNAs and cancer early diagnosis. Clin Transl Oncol. 2022;24(3):393–406. https://doi.org/10.1007/s12094-021-02706-6.
Dar GM, Agarwal S, Kumar A, Nimisha, Apurva, Sharma AK, et al. A non-invasive miRNA-based approach in early diagnosis and therapeutics of oral cancer. Crit Rev Oncol Hematol. 2022;180:103850. https://doi.org/10.1016/j.critrevonc.2022.103850.
DiStefano JK. miRNA profiling for the early detection and clinical monitoring of diabetic kidney disease. Biomark Med. 2017;11(2):99–102. https://doi.org/10.2217/bmm-2016-0301.
Galvão-Lima LJ, Morais AHF, Valentim RAM, Barreto E. miRNAs as biomarkers for early cancer detection and their application in the development of new diagnostic tools. Biomed Eng Online. 2021;20(1):21. https://doi.org/10.1186/s12938-021-00857-9.
Liu C, Xiang X, Han S, Lim HY, Li L, Zhang X, et al. Blood-based liquid biopsy: insights into early detection and clinical management of lung cancer. Cancer Lett. 2022;524:91–102. https://doi.org/10.1016/j.canlet.2021.10.013.
Rezayi M, Farjami Z, Hosseini ZS, Ebrahimi N, Abouzari-Lotf E. MicroRNA-based biosensors for early detection of cancers. Curr Pharm Des. 2018;24(39):4675–80. https://doi.org/10.2174/1381612825666190111144525.
Singh A, Dwivedi A. Circulating miRNA and cell-free DNA as a potential diagnostic tool in early detection of biliary tract cancer: a meta-analysis. Biomarkers. 2022;27(5):399–406. https://doi.org/10.1080/1354750x.2022.2064551.
Tarasiuk A, Mackiewicz T, Małecka-Panas E, Fichna J. Biomarkers for early detection of pancreatic cancer - miRNAs as a potential diagnostic and therapeutic tool? Cancer Biol Ther. 2021;22(5–6):347–56. https://doi.org/10.1080/15384047.2021.1941584.
Usuba W, Urabe F, Yamamoto Y, Matsuzaki J, Sasaki H, Ichikawa M, et al. Circulating miRNA panels for specific and early detection in bladder cancer. Cancer Sci. 2019;110(1):408–19. https://doi.org/10.1111/cas.13856.
Roth P, Keller A, Hoheisel JD, Codo P, Bauer AS, Backes C, et al. Differentially regulated miRNAs as prognostic biomarkers in the blood of primary CNS lymphoma patients. Eur J Cancer. 2015;51(3):382–90. https://doi.org/10.1016/j.ejca.2014.10.028.
Mao X, Sun Y, Tang J. Serum miR-21 is a diagnostic and prognostic marker of primary central nervous system lymphoma. Neurol Sci. 2014;35(2):233–8. https://doi.org/10.1007/s10072-013-1491-9.
Zhao HT, Chen J, Shi SB, Tian J, Tao RJ. Pemetrexed plus rituximab as second-line treatment for primary central nervous system lymphoma. Med Oncol. 2015;32(1):351. https://doi.org/10.1007/s12032-014-0351-7.
Takashima Y, Kawaguchi A, Iwadate Y, Hondoh H, Fukai J, Kajiwara K, et al. MicroRNA signature constituted of miR-30d, miR-93, and miR-181b is a promising prognostic marker in primary central nervous system lymphoma. PLoS One. 2019;14(1):e0210400. https://doi.org/10.1371/journal.pone.0210400.
Takashima Y, Kawaguchi A, Iwadate Y, Hondoh H, Fukai J, Kajiwara K, et al. miR-101, miR-548b, miR-554, and miR-1202 are reliable prognosis predictors of the miRNAs associated with cancer immunity in primary central nervous system lymphoma. PLoS One. 2020;15(2):e0229577. https://doi.org/10.1371/journal.pone.0229577.
Matera AG, Terns RM, Terns MP. Non-coding RNAs: lessons from the small nuclear and small nucleolar RNAs. Nat Rev Mol Cell Biol. 2007;8(3):209–20. https://doi.org/10.1038/nrm2124.
Newman A. Small nuclear RNAs and pre-mRNA splicing. Curr Opin Cell Biol. 1994;6(3):360–7. https://doi.org/10.1016/0955-0674(94)90027-2.
Shi J, Zhou T, Chen Q. Exploring the expanding universe of small RNAs. Nat Cell Biol. 2022;24(4):415–23. https://doi.org/10.1038/s41556-022-00880-5.
Baraniskin A, Zaslavska E, Nöpel-Dünnebacke S, Ahle G, Seidel S, Schlegel U, et al. Circulating U2 small nuclear RNA fragments as a novel diagnostic biomarker for primary central nervous system lymphoma. Neuro Oncol. 2016;18(3):361–7. https://doi.org/10.1093/neuonc/nov144.
Takashima Y, Sasaki Y, Hayano A, Homma J, Fukai J, Iwadate Y, et al. Target amplicon exome-sequencing identifies promising diagnosis and prognostic markers involved in RTK-RAS and PI3K-AKT signaling as central oncopathways in primary central nervous system lymphoma. Oncotarget. 2018;9(44):27471–86. https://doi.org/10.18632/oncotarget.25463.
Kim J, Kim TG, Lee HW, Kim SH, Park JE, Lee M, et al. Clinical outcomes of RTOG 9310 protocol for primary central nervous system lymphoma: single-center experience with 87 patients. Curr Oncol. 2021;28(6):4655–72. https://doi.org/10.3390/curroncol28060393.
Liu J, Wang Y, Liu Y, Liu Z, Cui Q, Ji N, et al. Immunohistochemical profile and prognostic significance in primary central nervous system lymphoma: Analysis of 89 cases. Oncol Lett. 2017;14(5):5505–12. https://doi.org/10.3892/ol.2017.6893.
Barakat M, Albitar M, Whitney R, Abdulhaq H. Diversity of genetic alterations of primary central nervous system lymphoma in Hispanic versus non-Hispanic patients. Cancer Treat Res Commun. 2021;27:100310. https://doi.org/10.1016/j.ctarc.2021.100310.
Alcoceba M, García-Álvarez M, Medina A, Maldonado R, González-Calle V, Chillón MC, et al. MYD88 mutations: transforming the landscape of IgM monoclonal gammopathies. Int J Mol Sci. 2022;23(10):5570. https://doi.org/10.3390/ijms23105570.
Eluard B, Nuan-Aliman S, Faumont N, Collares D, Bordereaux D, Montagne A, et al. The alternative RelB NF-κB subunit is a novel critical player in diffuse large B-cell lymphoma. Blood. 2022;139(3):384–98. https://doi.org/10.1182/blood.2020010039.
Gonzalez-Farre B, Ramis-Zaldivar JE, de CastrejónAnta N, Rivas-Delgado A, Nadeu F, Salmeron-Villalobos J, et al. Intravascular large B-cell lymphoma genomic profile is characterized by alterations in genes regulating NF-κB and immune checkpoints. Am J Surg Pathol. 2023;47(2):202–11. https://doi.org/10.1097/pas.0000000000001978.
Venturutti L, Rivas MA, Pelzer BW, Flümann R, Hansen J, Karagiannidis I, et al. An aged/autoimmune B-cell program defines the early transformation of extranodal lymphomas. Cancer Discov. 2023;13(1):216–43. https://doi.org/10.1158/2159-8290.Cd-22-0561.
Curran OE, Poon MTC, Gilroy L, Torgersen A, Smith C, Al-Qsous W. MYD88 L265P mutation in primary central nervous system lymphoma is associated with better survival: a single-center experience. Neurooncol Adv. 2021;3(1):vdab090. https://doi.org/10.1093/noajnl/vdab090.
Hattori K, Sakata-Yanagimoto M, Okoshi Y, Goshima Y, Yanagimoto S, Nakamoto-Matsubara R, et al. MYD88 (L265P) mutation is associated with an unfavourable outcome of primary central nervous system lymphoma. Br J Haematol. 2017;177(3):492–4. https://doi.org/10.1111/bjh.14080.
Takano S, Hattori K, Ishikawa E, Narita Y, Iwadate Y, Yamaguchi F, et al. MyD88 mutation in elderly predicts poor prognosis in primary central nervous system lymphoma: multi-institutional analysis. World Neurosurg. 2018;112:e69–73. https://doi.org/10.1016/j.wneu.2017.12.028.
Gupta M, Burns EJ, Georgantas NZ, Thierauf J, Nayyar N, Gordon A, et al. A rapid genotyping panel for detection of primary central nervous system lymphoma. Blood. 2021;138(5):382–6. https://doi.org/10.1182/blood.2020010137.
El Biali M, Karch R, Philippe C, Haslacher H, Tournier N, Hacker M, et al. ABCB1 and ABCG2 together limit the distribution of ABCB1/ABCG2 substrates to the human retina and the ABCG2 single nucleotide polymorphism q141k (c.421C>A) may lead to increased drug exposure. Front Pharmacol. 2021;12:698966. https://doi.org/10.3389/fphar.2021.698966.
Lin F, de Gooijer MC, Roig EM, Buil LC, Christner SM, Beumer JH, et al. ABCB1, ABCG2, and PTEN determine the response of glioblastoma to temozolomide and ABT-888 therapy. Clin Cancer Res. 2014;20(10):2703–13. https://doi.org/10.1158/1078-0432.Ccr-14-0084.
Sita G, Hrelia P, Tarozzi A, Morroni F. P-glycoprotein (ABCB1) and oxidative stress: focus on alzheimer’s disease. Oxid Med Cell Longev. 2017;2017:7905486. https://doi.org/10.1155/2017/7905486.
Wu T, Kang H, Zhuang D, Ma Y, Lin Z, Suolitiken D, et al. The role of ABCB1 polymorphism as a prognostic marker for primary central nervous system lymphoma. Ann Hematol. 2019;98(4):923–30. https://doi.org/10.1007/s00277-019-03629-7.
Gong Y, Luo L, Wang L, Chen J, Chen F, Ma Y, et al. Association of MTHFR and ABCB1 polymorphisms with MTX-induced mucositis in Chinese paediatric patients with acute lymphoblastic leukaemia, lymphoma or osteosarcoma-A retrospective cohort study. J Clin Pharm Ther. 2021;46(6):1557–63. https://doi.org/10.1111/jcpt.13505.
Esmaili MA, Kazemi A, Faranoush M, Mellstedt H, Zaker F, Safa M, et al. Polymorphisms within methotrexate pathway genes: Relationship between plasma methotrexate levels, toxicity experienced and outcome in pediatric acute lymphoblastic leukemia. Iran J Basic Med Sci. 2020;23(6):800–9. https://doi.org/10.22038/ijbms.2020.41754.9858.
Kunishio K, Nagao S. Prognostic implication of p27 expression in primary central nervous system lymphoma. Brain Tumor Pathol. 2006;23(2):77–81. https://doi.org/10.1007/s10014-006-0206-9.
Audia JE, Campbell RM. Histone modifications and cancer. Cold Spring Harb Perspect Biol. 2016;8(4):a019521. https://doi.org/10.1101/cshperspect.a019521.
Kim HG, Kim MS, Lee YS, Lee EH, Kim DC, Lee SH, et al. Hypo-trimethylation of histone H3 lysine 4 and hyper-tri/dimethylation of histone H3 lysine 27 as epigenetic markers of poor prognosis in patients with primary central nervous system lymphoma. Cancer Res Treat. 2022;54(3):690–708. https://doi.org/10.4143/crt.2021.1121.
Takashima Y, Kawaguchi A, Sato R, Yoshida K, Hayano A, Homma J, et al. Differential expression of individual transcript variants of PD-1 and PD-L2 genes on Th-1/Th-2 status is guaranteed for prognosis prediction in PCNSL. Sci Rep. 2019;9(1):10004. https://doi.org/10.1038/s41598-019-46473-5.
Cho H, Kim SH, Kim SJ, Chang JH, Yang WI, Suh CO, et al. Programmed cell death 1 expression is associated with inferior survival in patients with primary central nervous system lymphoma. Oncotarget. 2017;8(50):87317–28. https://doi.org/10.18632/oncotarget.20264.
Cho I, Lee H, Yoon SE, Ryu KJ, Ko YH, Kim WS, et al. Serum levels of soluble programmed death-ligand 1 (sPD-L1) in patients with primary central nervous system diffuse large B-cell lymphoma. BMC Cancer. 2020;20(1):120. https://doi.org/10.1186/s12885-020-6612-2.
Furuse M, Kuwabara H, Ikeda N, Hattori Y, Ichikawa T, Kagawa N, et al. PD-L1 and PD-L2 expression in the tumor microenvironment including peritumoral tissue in primary central nervous system lymphoma. BMC Cancer. 2020;20(1):277. https://doi.org/10.1186/s12885-020-06755-y.
Parkhi M, Chatterjee D, Bal A, Vias P, Yadav BS, Prakash G, et al. Prognostic implications of the tumor immune microenvironment and immune checkpoint pathway in primary central nervous system diffuse large B-cell lymphoma in the North Indian population. APMIS. 2022;130(2):82–94. https://doi.org/10.1111/apm.13195.
Li X, He X, Xu X, Song Z, Qian C, Wang J, et al. The potential role of Ku80 in primary central nervous system lymphoma as a prognostic factor. Contemp Oncol (Pozn). 2013;17(1):58–63. https://doi.org/10.5114/wo.2013.33775.
Bai S, Zhu W, Coffman L, Vlad A, Schwartz LE, Elishaev E, et al. CD105 is expressed in ovarian cancer precursor lesions and is required for metastasis to the ovary. Cancers (Basel). 2019;11(11):1710. https://doi.org/10.3390/cancers11111710.
Benetti A, Berenzi A, Gambarotti M, Garrafa E, Gelati M, Dessy E, et al. Transforming growth factor-beta1 and CD105 promote the migration of hepatocellular carcinoma-derived endothelium. Cancer Res. 2008;68(20):8626–34. https://doi.org/10.1158/0008-5472.Can-08-1218.
Duff SE, Li C, Garland JM, Kumar S. CD105 is important for angiogenesis: evidence and potential applications. Faseb j. 2003;17(9):984–92. https://doi.org/10.1096/fj.02-0634rev.
Kasprzak A, Adamek A. Role of Endoglin (CD105) in the progression of hepatocellular carcinoma and anti-angiogenic therapy. Int J Mol Sci. 2018;19(12):3887. https://doi.org/10.3390/ijms19123887.
Kong X, Wang Y, Liu S, Xing B, Yang Y, Li Y, et al. CD105 over-expression Is associated with higher WHO grades for gliomas. Mol Neurobiol. 2016;53(5):3503–12. https://doi.org/10.1007/s12035-015-9677-1.
Oladejo M, Nguyen HM, Seah H, Datta A, Wood LM. Tumoral CD105 promotes immunosuppression, metastasis, and angiogenesis in renal cell carcinoma. Cancer Immunol Immunother. 2023;72(6):1633–46. https://doi.org/10.1007/s00262-022-03356-5.
Sier VQ, van der Vorst JR, Quax PHA, de Vries MR, Zonoobi E, Vahrmeijer AL, et al. Endoglin/CD105-based imaging of cancer and cardiovascular diseases: a systematic review. Int J Mol Sci. 2021;22(9):4804. https://doi.org/10.3390/ijms22094804.
Sugita Y, Takase Y, Mori D, Tokunaga O, Nakashima A, Shigemori M. Endoglin (CD105) is expressed on endothelial cells in the primary central nervous system lymphomas and correlates with survival. J Neurooncol. 2007;82(3):249–56. https://doi.org/10.1007/s11060-006-9281-3.
Abdel-Wahab AF, Mahmoud W, Al-Harizy RM. Targeting glucose metabolism to suppress cancer progression: prospective of anti-glycolytic cancer therapy. Pharmacol Res. 2019;150:104511. https://doi.org/10.1016/j.phrs.2019.104511.
Dong S, Li W, Li X, Wang Z, Chen Z, Shi H, et al. Glucose metabolism and tumour microenvironment in pancreatic cancer: A key link in cancer progression. Front Immunol. 2022;13:1038650. https://doi.org/10.3389/fimmu.2022.1038650.
Gyamfi J, Kim J, Choi J. Cancer as a metabolic disorder. Int J Mol Sci. 2022;23(3):1155. https://doi.org/10.3390/ijms23031155.
Hay N. Reprogramming glucose metabolism in cancer: can it be exploited for cancer therapy? Nat Rev Cancer. 2016;16(10):635–49. https://doi.org/10.1038/nrc.2016.77.
Vander Heiden MG, Cantley LC, Thompson CB. Understanding the Warburg effect: the metabolic requirements of cell proliferation. Science. 2009;324(5930):1029–33. https://doi.org/10.1126/science.1160809.
Zhao H, Li Y. Cancer metabolism and intervention therapy. Mol Biomed. 2021;2(1):5. https://doi.org/10.1186/s43556-020-00012-1.
You M, Xie Z, Zhang N, Zhang Y, Xiao D, Liu S, et al. Signaling pathways in cancer metabolism: mechanisms and therapeutic targets. Signal Transduct Target Ther. 2023;8(1):196. https://doi.org/10.1038/s41392-023-01442-3.
Takashima Y, Hayano A, Yamanaka R. Metabolome analysis reveals excessive glycolysis via PI3K/AKT/mTOR and RAS/MAPK signaling in methotrexate-resistant primary CNS lymphoma-derived cells. Clin Cancer Res. 2020;26(11):2754–66. https://doi.org/10.1158/1078-0432.Ccr-18-3851.
Kim JA, Kim SJ, Do IG, Jin J, Nam DH, Ko YH, et al. Hypoxia-associated protein expression in primary central nervous system diffuse large B-cell lymphoma: does it predict prognosis? Leuk Lymphoma. 2011;52(2):205–13. https://doi.org/10.3109/10428194.2010.542261.
Debata A, Yoshida K, Ujifuku K, Yasui H, Kamada K, Niino D, et al. Hyperglycemia is associated with poor survival in primary central nervous system lymphoma patients. Tumori. 2017;103(3):272–8. https://doi.org/10.5301/tj.5000590.
Zhang X, Wu Y, Sun X, Cui Q, Bai X, Dong G, et al. The PI3K/AKT/mTOR signaling pathway is aberrantly activated in primary central nervous system lymphoma and correlated with a poor prognosis. BMC Cancer. 2022;22(1):190. https://doi.org/10.1186/s12885-022-09275-z.
Chen J, Ge X, Zhang W, Ding P, Du Y, Wang Q, et al. PI3K/AKT inhibition reverses R-CHOP resistance by destabilizing SOX2 in diffuse large B cell lymphoma. Theranostics. 2020;10(7):3151–63. https://doi.org/10.7150/thno.41362.
Damodaran S, Zhao F, Deming DA, Mitchell EP, Wright JJ, Gray RJ, et al. Phase II study of copanlisib in patients with tumors with PIK3CA mutations: results from the NCI-MATCH ECOG-ACRIN Trial (EAY131) subprotocol Z1F. J Clin Oncol. 2022;40(14):1552–61. https://doi.org/10.1200/jco.21.01648.
Xu W, Berning P, Lenz G. Targeting B-cell receptor and PI3K signaling in diffuse large B-cell lymphoma. Blood. 2021;138(13):1110–9. https://doi.org/10.1182/blood.2020006784.
Yang J, Li Y, Zhang Y, Fang X, Chen N, Zhou X, et al. SIRT6 promotes tumorigenesis and drug resistance of diffuse large B-cell lymphoma by mediating PI3K/Akt signaling. J Exp Clin Cancer Res. 2020;39(1):142. https://doi.org/10.1186/s13046-020-01623-w.
Cao W, Liu J, Jiang Z, Tao Y, Wang H, Li J, et al. Tumor suppressor adenomatous polyposis coli sustains dendritic cell tolerance through IL-10 in a β-catenin-dependent manner. J Immunol. 2023;210(10):1589–97. https://doi.org/10.4049/jimmunol.2300046.
Hansson C, Lebrero-Fernández C, Schön K, Angeletti D, Lycke N. Tr1 cell-mediated protection against autoimmune disease by intranasal administration of a fusion protein targeting cDC1 cells. Mucosal Immunol. 2023. https://doi.org/10.1016/j.mucimm.2023.05.006.
Kak G, Van Roy Z, Heim CE, Fallet RW, Shi W, Roers A, et al. IL-10 production by granulocytes promotes Staphylococcus aureus craniotomy infection. J Neuroinflammation. 2023;20(1):114. https://doi.org/10.1186/s12974-023-02798-7.
Monjaras-Avila CU, Lorenzo-Leal AC, Luque-Badillo AC, D'Costa N, Chavez-Muñoz C, Bach H. The tumor immune microenvironment in clear cell renal cell carcinoma. Int J Mol Sci. 2023;24(9). https://doi.org/10.3390/ijms24097946.
Geginat J, Vasco M, Gerosa M, Tas SW, Pagani M, Grassi F, et al. IL-10 producing regulatory and helper T-cells in systemic lupus erythematosus. Semin Immunol. 2019;44:101330. https://doi.org/10.1016/j.smim.2019.101330.
Moore KW, de Waal MR, Coffman RL, O’Garra A. Interleukin-10 and the interleukin-10 receptor. Annu Rev Immunol. 2001;19:683–765. https://doi.org/10.1146/annurev.immunol.19.1.683.
Zhang H, Li R, Cao Y, Gu Y, Lin C, Liu X, et al. Poor clinical outcomes and immunoevasive contexture in intratumoral IL-10-producing macrophages enriched gastric cancer patients. Ann Surg. 2022;275(4):e626–35. https://doi.org/10.1097/sla.0000000000004037.
Sasayama T, Nakamizo S, Nishihara M, Kawamura A, Tanaka H, Mizukawa K, et al. Cerebrospinal fluid interleukin-10 is a potentially useful biomarker in immunocompetent primary central nervous system lymphoma (PCNSL). Neuro Oncol. 2012;14(3):368–80. https://doi.org/10.1093/neuonc/nor203.
Mizowaki T, Sasayama T, Tanaka K, Mizukawa K, Takata K, Nakamizo S, et al. STAT3 activation is associated with cerebrospinal fluid interleukin-10 (IL-10) in primary central nervous system diffuse large B cell lymphoma. J Neurooncol. 2015;124(2):165–74. https://doi.org/10.1007/s11060-015-1843-9.
Nguyen-Them L, Costopoulos M, Tanguy ML, Houillier C, Choquet S, Benanni H, et al. The CSF IL-10 concentration is an effective diagnostic marker in immunocompetent primary CNS lymphoma and a potential prognostic biomarker in treatment-responsive patients. Eur J Cancer. 2016;61:69–76. https://doi.org/10.1016/j.ejca.2016.03.080.
Geng M, Song Y, Xiao H, Wu Z, Deng X, Chen C, et al. Clinical significance of interleukin-10 concentration in the cerebrospinal fluid of patients with primary central nervous system lymphoma. Oncol Lett. 2021;21(1):2. https://doi.org/10.3892/ol.2020.12263.
Sasayama T, Tanaka K, Mizowaki T, Nagashima H, Nakamizo S, Tanaka H, et al. Tumor-associated macrophages associate with cerebrospinal fluid interleukin-10 and survival in primary central nervous system lymphoma (PCNSL). Brain Pathol. 2016;26(4):479–87. https://doi.org/10.1111/bpa.12318.
Hayano A, Komohara Y, Takashima Y, Takeya H, Homma J, Fukai J, et al. Programmed cell death ligand 1 expression in primary central nervous system lymphomas: a clinicopathological study. Anticancer Res. 2017;37(10):5655–66. https://doi.org/10.21873/anticanres.12001.
Vater I, Montesinos-Rongen M, Schlesner M, Haake A, Purschke F, Sprute R, et al. The mutational pattern of primary lymphoma of the central nervous system determined by whole-exome sequencing. Leukemia. 2015;29(3):677–85. https://doi.org/10.1038/leu.2014.264.
Hu C, Jiang W, Lv M, Fan S, Lu Y, Wu Q, et al. Potentiality of exosomal proteins as novel cancer biomarkers for liquid biopsy. Front Immunol. 2022;13:792046. https://doi.org/10.3389/fimmu.2022.792046.
Takashima Y, Yoshimura T, Kano Y, Hayano A, Hondoh H, Ikenaka K, et al. Differential expression of N-linked oligosaccharides in methotrexate-resistant primary central nervous system lymphoma cells. BMC Cancer. 2019;19(1):910. https://doi.org/10.1186/s12885-019-6129-8.
Hayano A, Takashima Y, Yamanaka R. Cell-type-specific sensitivity of bortezomib in the methotrexate-resistant primary central nervous system lymphoma cells. Int J Clin Oncol. 2019;24(9):1020–9. https://doi.org/10.1007/s10147-019-01451-9.
Gandhi MK, Khanna R. Viruses and lymphoma. Pathology. 2005;37(6):420–33. https://doi.org/10.1080/003130200500368303.
Kawano T, Inokuchi J, Eto M, Murata M, Kang JH. Activators and inhibitors of protein kinase C (PKC): their applications in clinical trials. Pharmaceutics. 2021;13(11):1748. https://doi.org/10.3390/pharmaceutics13111748.
Hatic H, Sampat D, Goyal G. Immune checkpoint inhibitors in lymphoma: challenges and opportunities. Ann Transl Med. 2021;9(12):1037. https://doi.org/10.21037/atm-20-6833.
Acknowledgements
We thank the members of You’s lab for helpful discussions.
Funding
This study was supported by the National Natural Science Foundation of China (82203844, 82203213, 81911530169), Basic and Applied Basic Research Project of Guangdong Province (2020A1515111201 and 2021A1515010083), University Special Innovative Research Program of Department of Education of Guangdong Province (2020KQNCX073), CQMU Program for Youth Innovation in Future Medicine (W0202), Talent Program of Chongqing Health Commission.
Author information
Authors and Affiliations
Contributions
Hua Yang and YX contributed equally to the work. Hua You conceived the hypothesis. Hua Yang, CK, KT and Hua You revised the manuscript. Hua Yang and YX, did the literature search and wrote the manuscript. Hua Yang and Hua You prepared the tables and figures. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Ethical Approval is not applicable. This paper has not been published elsewhere in whole or in part. All authors have read and approved the content, and agree to submit it for consideration for publication.
Consent for publication
Consent for publication is not applicable in this research.
Competing interests
The authors declare no competing interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yang, H., Xun, Y., Ke, C. et al. Extranodal lymphoma: pathogenesis, diagnosis and treatment. Mol Biomed 4, 29 (2023). https://doi.org/10.1186/s43556-023-00141-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s43556-023-00141-3